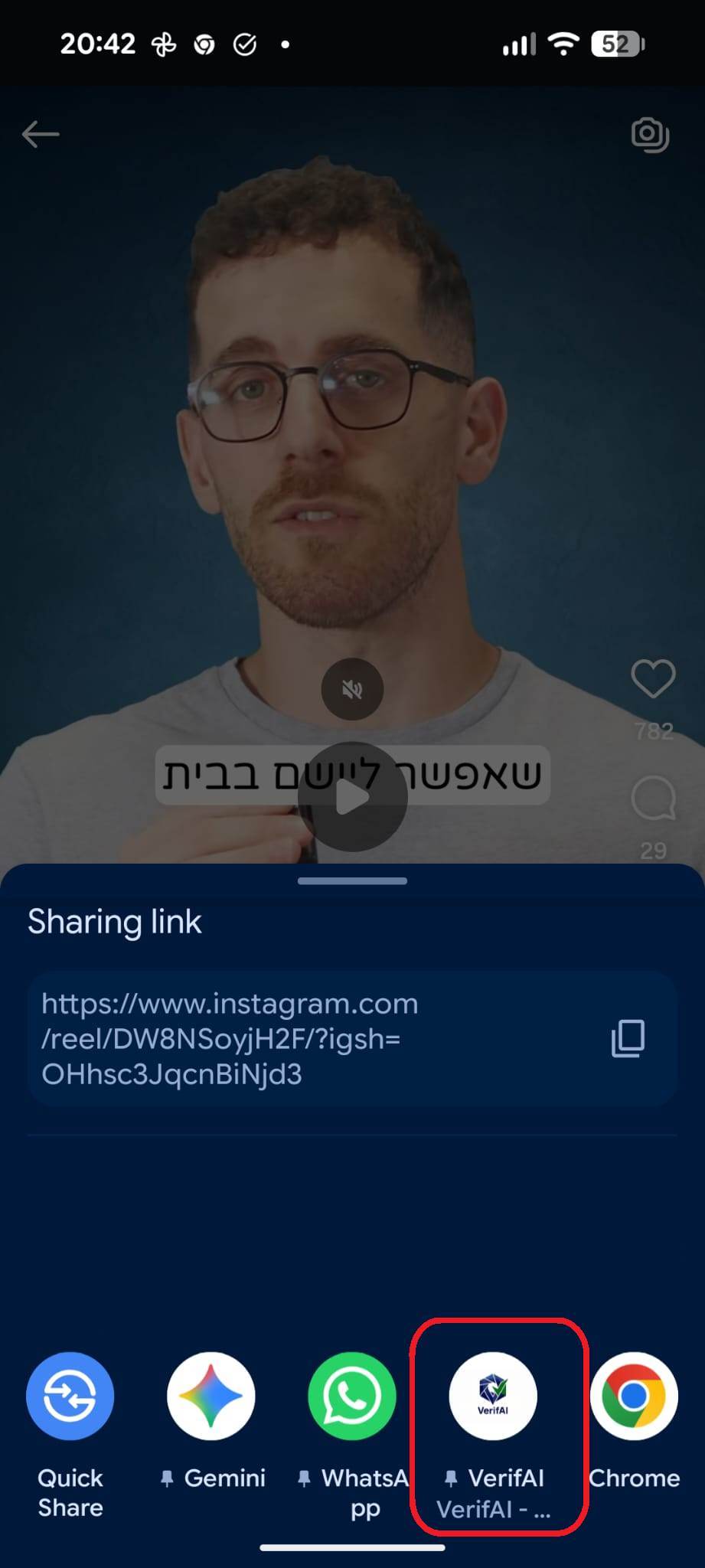
סריקה בתהליך...
הניתוח עשוי לארוך 30–90 שניות
הידעת?
הסרטון אינו מכיל תוכן רפואי
חושבים שחלה טעות?
אם לדעתכם הסרטון אכן עוסק בטענות רפואיות או בריאותיות, הוסיפו הסבר קצר ושלחו בקשה לבדיקה מחדש.
הבקשה התקבלה! נבדוק את הסרטון ונחזור אליכם.
אירעה שגיאה בשליחת הבקשה. נסו שוב.
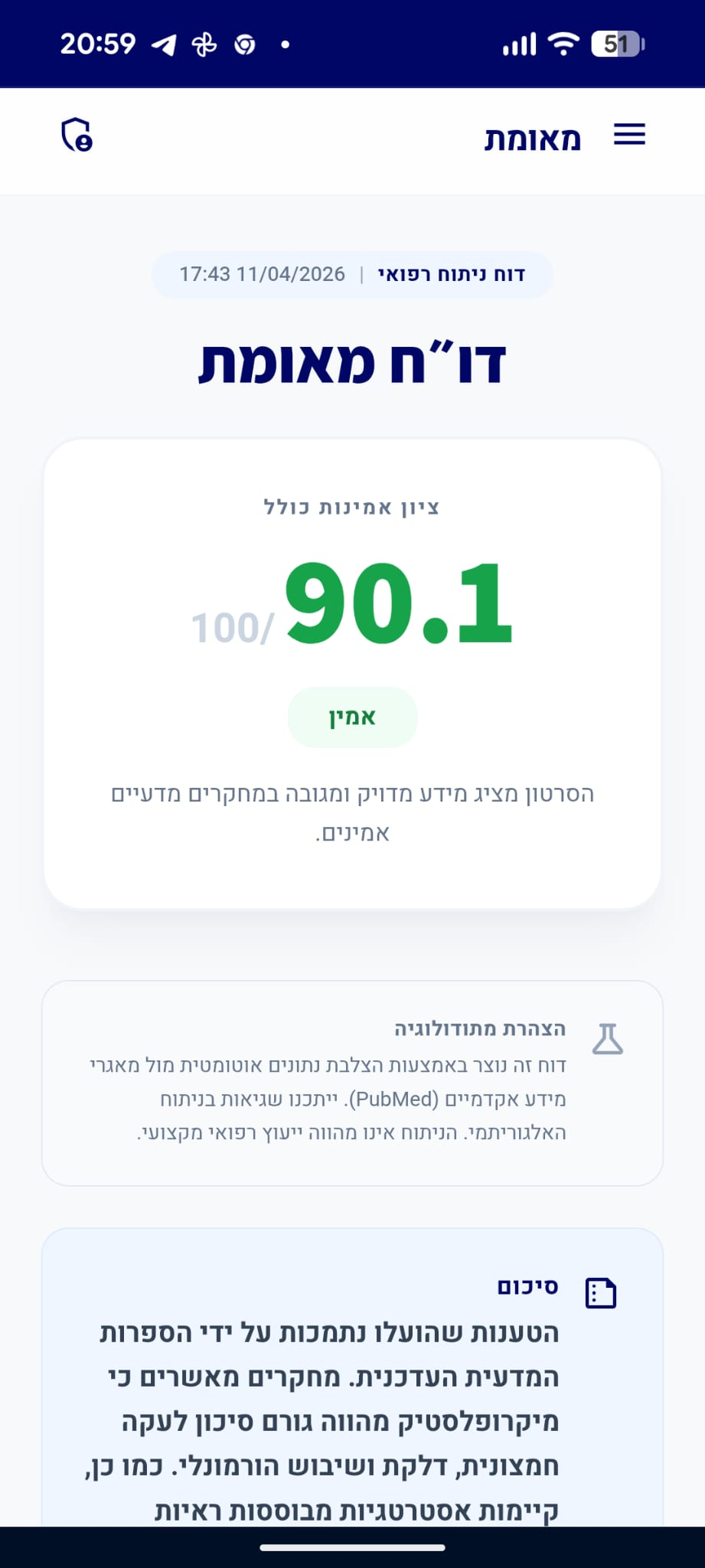
דו״ח מאומת
הסרטון מציג מידע מדויק ומגובה במחקרים מדעיים אמינים.
סיכום
הטענות שהוצגו משקפות ברובן את הקונצנזוס המדעי הנוכחי. בעוד שהקשר בין בשר אדום לא מעובד למחלות לב נותר נושא לדיון מדעי בשל ממצאים סותרים, ישנה הסכמה רחבה יותר בספרות המדעית לגבי ההשפעות המיטיבות של החלפת בשר אדום בחלבון צמחי, והסיכון המוגבר הקשור לצריכת בשר מעובד.
analytics ניתוח טענות מבוסס ראיות
"צריכת בשר אדום אינה מעלה משמעותית את הסיכון למחלות לב וכלי דם."
מסקנת הבדיקה:
הספרות המדעית מציגה ממצאים לא עקביים בנוגע לקשר בין צריכת בשר אדום לבין מחלות לב וכלי דם. בעוד שמחקרים תצפיתיים מסוימים מצביעים על קשר אפשרי, מטא-אנליזות של מחקרים מבוקרים (RCTs) לא מצאו השפעה מובהקת וחד-משמעית המצדיקה קביעה גורפת. (🟨)
chevron_right מקורות מדעיים: (4)
-
link
Red meat consumption, cardiovascular diseases, and diabetes: a systematic review and meta-analysis.
Observational studies show inconsistent associations of red meat consumption with cardiovascular disease (CVD) and diabetes. Moreover, red meat consumption varies by sex and setting, however, whether the associations vary by sex and setting remains unclear. This systematic review and meta-analysis was conducted to summarize the evidence concerning the associations of unprocessed and processed red meat consumption with CVD and its subtypes [coronary heart disease (CHD), stroke, and heart failure], type two diabetes mellitus (T2DM), and gestational diabetes mellitus (GDM) and to assess differences by sex and setting (western vs. eastern, categorized based on dietary pattern and geographic region). Two researchers independently screened studies from PubMed, Web of Science, Embase, and the Cochrane Library for observational studies and randomized controlled trials (RCTs) published by 30 June 2022. Forty-three observational studies (N = 4 462 810, 61.7% women) for CVD and 27 observational studies (N = 1 760 774, 64.4% women) for diabetes were included. Red meat consumption was positively associated with CVD [hazard ratio (HR) 1.11, 95% confidence interval (CI) 1.05 to 1.16 for unprocessed red meat (per 100 g/day increment); 1.26, 95% CI 1.18 to 1.35 for processed red meat (per 50 g/day increment)], CVD subtypes, T2DM, and GDM. The associations with stroke and T2DM were higher in western settings, with no difference by sex. Unprocessed and processed red meat consumption are both associated with higher risk of CVD, CVD subtypes, and diabetes, with a stronger association in western settings but no sex difference. Better understanding of the mechanisms is needed to facilitate improving cardiometabolic and planetary health.…
PMID: 37264855
-
link
Meta-Analysis of Randomized Controlled Trials of Red Meat Consumption in Comparison With Various Comparison Diets on Cardiovascular Risk Factors.
Findings among randomized controlled trials evaluating the effect of red meat on cardiovascular disease risk factors are inconsistent. We provide an updated meta-analysis of randomized controlled trials on red meat and cardiovascular risk factors and determine whether the relationship depends on the composition of the comparison diet, hypothesizing that plant sources would be relatively beneficial. We conducted a systematic PubMed search of randomized controlled trials published up until July 2017 comparing diets with red meat with diets that replaced red meat with a variety of foods. We stratified comparison diets into high-quality plant protein sources (legumes, soy, nuts); chicken/poultry/fish; fish only; poultry only; mixed animal protein sources (including dairy); carbohydrates (low-quality refined grains and simple sugars, such as white bread, pasta, rice, cookies/biscuits); or usual diet. We performed random-effects meta-analyses comparing differences in changes of blood lipids, apolipoproteins, and blood pressure for all studies combined and stratified by specific comparison diets. Thirty-six studies totaling 1803 participants were included. There were no significant differences between red meat and all comparison diets combined for changes in blood concentrations of total, low-density lipoprotein, or high-density lipoprotein cholesterol, apolipoproteins A1 and B, or blood pressure. Relative to the comparison diets combined, red meat resulted in lesser decreases in triglycerides (weighted mean difference [WMD], 0.065 mmol/L; 95% CI, 0.000-0.129; P for heterogeneity <0.01). When analyzed by specific comparison diets, relative to high-quality plant protein sources, red meat yielded lesser decreases in total cholesterol (WMD, 0.264 mmol/L; 95% CI, 0.144-0.383; P<0.001) and low-density lipoprotein (WMD, 0.198 mmol/L; 95% CI, 0.065-0.330; P=0.003). In comparison with fish, red meat yielded greater decreases in low-density lipoprotein (WMD, -0.173 mmol/L; 95% CI, -0.260 to -0.086; P<0.001) and high-density lipoprotein (WMD, -0.065 mmol/L; 95% CI, -0.109 to -0.020; P=0.004). In comparison with carbohydrates, red meat yielded greater decreases in triglycerides (WMD, -0.181 mmol/L; 95% CI, -0.349 to -0.013). Inconsistencies regarding the effects of red meat on cardiovascular disease risk factors are attributable, in part, to the composition of the comparison diet. Substituting red meat with high-quality plant protein sources, but not with fish or low-quality carbohydrates, leads to more favorable changes in blood lipids and lipoproteins.…
PMID: 30958719
-
link
Red and Processed Meat Consumption and Risk for All-Cause Mortality and Cardiometabolic Outcomes: A Systematic Review and Meta-analysis of Cohort Studies.
This article has been corrected. The original version (PDF) is appended to this article as a Supplement. Dietary guidelines generally recommend limiting intake of red and processed meat. However, the quality of evidence implicating red and processed meat in adverse health outcomes remains unclear. To evaluate the association between red and processed meat consumption and all-cause mortality, cardiometabolic outcomes, quality of life, and satisfaction with diet among adults. EMBASE (Elsevier), Cochrane Central Register of Controlled Trials (Wiley), Web of Science (Clarivate Analytics), CINAHL (EBSCO), and ProQuest from inception until July 2018 and MEDLINE from inception until April 2019, without language restrictions, as well as bibliographies of relevant articles. Cohort studies with at least 1000 participants that reported an association between unprocessed red or processed meat intake and outcomes of interest. Teams of 2 reviewers independently extracted data and assessed risk of bias. One investigator assessed certainty of evidence, and the senior investigator confirmed the assessments. Of 61 articles reporting on 55 cohorts with more than 4 million participants, none addressed quality of life or satisfaction with diet. Low-certainty evidence was found that a reduction in unprocessed red meat intake of 3 servings per week is associated with a very small reduction in risk for cardiovascular mortality, stroke, myocardial infarction (MI), and type 2 diabetes. Likewise, low-certainty evidence was found that a reduction in processed meat intake of 3 servings per week is associated with a very small decrease in risk for all-cause mortality, cardiovascular mortality, stroke, MI, and type 2 diabetes. Inadequate adjustment for known confounders, residual confounding due to observational design, and recall bias associated with dietary measurement. The magnitude of association between red and processed meat consumption and all-cause mortality and adverse cardiometabolic outcomes is very small, and the evidence is of low certainty. None. (PROSPERO: CRD42017074074).…
PMID: 31569213
-
link
Red Meat Consumption and Risk of Cardio-Cerebrovascular Disease in Chinese Older Adults.
Associations between red meat consumption and cardio-cerebrovascular diseases (CCVDs) are mostly studied in Western populations but not in Chinese or elderly. This prospective study investigated adults ≥65 years from the China Kadoorie Biobank (CKB). Associations between red meat consumption and CCVD, ischemic stroke/transient ischemic attack (TIA), CCVD mortality, and all-cause mortality were determined by Cox regression. A total of 59,980 participants were analyzed, 14,715 (24.53%) of whom ate red meat daily, 9,843 (16.41%) ate red meat 4-6 days/week, 23,472 (39.13%) ate red meat 1-3 days/week, and 11,950 (19.92%) ate red meat less than 1 day/week. Average amount of red meat usual consumption was 38 g/day. After adjustment, per 50 g/day higher red meat consumption at baseline was significantly associated with increased incident CCVD (aHR = 1.10) among high-income subjects (≥ 10,000 RMB) and urban residents (aHR = 1.12). Per 50 g/day higher baseline red meat consumption was significantly associated with increased ischemic stroke/TIA in urban residents (aHR = 1.08) but decreased risk in rural residents (aHR = 0.84). Higher baseline red meat consumption was associated with lower CCVD mortality in the poorest (aHR = 0.78) and rural residents (aHR = 0.72) and lower all-cause mortality in the poorest (aHR = 0.82) and rural residents (aHR = 0.80). In general, among older adults in China, higher red meat intake independently predicted increased CCVD among urban and high-income individuals but not poor ones. Higher red meat intake appears to be protective against mortality in rural and low-income subjects. Socioeconomic status is a crucial modifying factor on the association between red meat consumption and adverse cardiovascular outcomes in China.…
PMID: 37518346
"במחקרים מבוקרים (RCTs), צריכת בשר אדום לא מעובד לא הראתה השפעה משמעותית על משקל או שומן גוף."
מסקנת הבדיקה:
מטא-אנליזות של מחקרים מבוקרים (RCTs) מצביעות על כך שצריכת בשר אדום לא מעובד אינה מובילה להשפעה מובהקת על מדדי משקל או הרכב גוף בהשוואה לקבוצות ביקורת במחקרים קליניים. (🟩)
"החלפת בשר אדום במקורות חלבון צמחיים עשויה לשפר מדדי בריאות לב וכלי דם."
מסקנת הבדיקה:
מחקרים קליניים ומודלים תזונתיים מראים כי החלפת בשר אדום במקורות חלבון צמחיים עשויה להוביל לשיפור במדדים מטבוליים וקרדיווסקולריים, כגון רמות כולסטרול ורגישות לאינסולין. (🟩)
chevron_right מקורות מדעיים: (3)
-
link
The effects of substituting red and processed meat for mycoprotein on biomarkers of cardiovascular risk in healthy volunteers: an analysis of secondary endpoints from Mycomeat.
Mycoprotein is a relatively novel food source produced from the biomass of Fusarium venenatum. It has previously been shown to improve CVD risk markers in intervention trials when it is compared against total meat. It has not hitherto been assessed specifically for benefits relative to red and processed meat. We leveraged samples from Mycomeat, an investigator-blind randomised crossover controlled trial in metabolically healthy male adults (n = 20), randomised to consume 240 g/day of red and processed meat for 14 days followed by mycoprotein, or vice versa. Blood biochemical indices were a priori defined secondary endpoints. Mycoprotein consumption led to a 6.74% reduction in total cholesterol (P = 0.02) and 12.3% reduction in LDL cholesterol (P = 0.02) from baseline values. Change in fasted triglycerides was not significantly different between diets (+ 0.19 ± 0.11 mmol/l with mycoprotein, P = 0.09). There was a small but significant reduction in waist circumference for mycoprotein relative to meat (- 0.95 ± 0.42 cm, P = 0.04). Following the mycoprotein diet, mean systolic (- 2.41 ± 1.89 mmHg, P = 0.23) and diastolic blood pressure (- 0.80 ± 1.23 mmHg, P = 0.43) were reduced from baseline. There were no statistically significant effects of the intervention on urinary sodium, nitrite or TMAO; while urinary potassium (+ 126.12 ± 50.30 mmol/l, P = 0.02) and nitrate (+ 2.12 ± 0.90 mmol/l, P = 0.04) were both significantly higher with mycoprotein relative to meat. The study population comprised metabolically healthy adults, therefore, changes in plasma lipids had little effect on cardiovascular risk scores (- 0.34% FRS for mycoprotein P = 0.24). These results confirm potential cardiovascular benefits when displacing red and processed meat with mycoprotein in the diet. Longer trials in higher risk study populations are needed to fully elucidate suggested benefits for blood pressure and body composition. gov Identifier: NCT03944421.…
PMID: 37624376
-
link
The Isocaloric Substitution of Plant-Based and Animal-Based Protein in Relation to Aging-Related Health Outcomes: A Systematic Review.
Plant-based and animal-based protein intake have differential effects on various aging-related health outcomes, but less is known about the health effect of isocaloric substitution of plant-based and animal-based protein. This systematic review summarized current evidence of the isocaloric substitutional effect of plant-based and animal-based protein on aging-related health outcomes. PubMed and Embase databases were searched for epidemiologic observational studies published in English up to 15 March 2021. Studies that included adults ≥18 years old; use of a nutritional substitution model to define isocaloric substitution of plant protein and animal protein; health outcomes covering mortality, aging-related diseases or indices; and reported association estimates with corresponding 95% confidence intervals were included. Nine cohort studies and 3 cross-sectional studies were identified, with a total of 1,450,178 subjects included in this review. Consistent and significant inverse association of substituting plant protein for various animal proteins on all-cause mortality was observed among 4 out of 5 studies with relative risks (RRs) from 0.54 to 0.95 and on cardiovascular disease (CVD) mortality among all 4 studies with RRs from 0.58 to 0.91. Among specific animal proteins, the strongest inverse association on all-cause and CVD mortality was identified when substituting plant protein for red and/or processed meat protein, with the effect mainly limited to bread, cereal, and pasta protein when replacing red meat protein. Isocaloric substitution of plant-based protein for animal-based protein might prevent all-cause and CVD-specific mortality. More studies are needed on this topic, particularly for cancer incidence and other specific aging-related diseases.…
PMID: 35057453
-
link
Modelling the replacement of red and processed meat with plant-based alternatives and the estimated effect on insulin sensitivity in a cohort of Australian adults.
Dietary guidelines are increasingly promoting mostly plant-based diets, limits on red meat consumption, and plant-based sources of protein for health and environmental reasons. It is unclear how the resulting food substitutions associate with insulin resistance, a risk factor for type 2 diabetes. We modelled the replacement of red and processed meat with plant-based alternatives and the estimated effect on insulin sensitivity. We included 783 participants (55 % female) from the Childhood Determinants of Adult Health study, a population-based cohort of Australians. In adulthood, diet was assessed at three time points using FFQ: 2004–2006, 2009–2011 and 2017–2019. We calculated the average daily intake of each food group in standard serves. Insulin sensitivity was estimated from fasting glucose and insulin concentrations in 2017–2019 (aged 39–49 years) using homoeostasis model assessment. Replacing red meat with a combination of plant-based alternatives was associated with higher insulin sensitivity (…
PMID: 37981891
"צריכה גבוהה של בשר מעובד או שומני מעלה את הסיכון למחלות לב."
מסקנת הבדיקה:
קיימות ראיות מדעיות המצביעות על קשר בין צריכה גבוהה של בשר מעובד לבין עלייה בסיכון למחלות לב איסכמיות, בהתבסס על מחקרי עוקבה ומטא-אנליזות רחבות היקף. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
Health effects associated with consumption of processed meat, sugar-sweetened beverages and trans fatty acids: a Burden of Proof study.
Previous research suggests detrimental health effects associated with consuming processed foods, including processed meats, sugar-sweetened beverages (SSBs) and trans fatty acids (TFAs). However, systematic characterization of the dose-response relationships between these foods and health outcomes is limited. Here, using Burden of Proof meta-regression methods, we evaluated the associations between processed meat, SSBs and TFAs and three chronic diseases: type 2 diabetes, ischemic heart disease (IHD) and colorectal cancer. We conservatively estimated that-relative to zero consumption-consuming processed meat (at 0.6-57 g d…
PMID: 40588677
-
link
Consumption of Meat, Fish, Dairy Products, and Eggs and Risk of Ischemic Heart Disease.
There is uncertainty about the relevance of animal foods to the pathogenesis of ischemic heart disease (IHD). We examined meat, fish, dairy products, and eggs and risk for IHD in the pan-European EPIC cohort (European Prospective Investigation Into Cancer and Nutrition). In this prospective study of 409 885 men and women in 9 European countries, diet was assessed with validated questionnaires and calibrated with 24-hour recalls. Lipids and blood pressure were measured in a subsample. During a mean of 12.6 years of follow-up, 7198 participants had a myocardial infarction or died of IHD. The relationships of animal foods with risk were examined with Cox regression with adjustment for other animal foods and relevant covariates. The hazard ratio (HR) for IHD was 1.19 (95% CI, 1.06-1.33) for a 100-g/d increment in intake of red and processed meat, and this remained significant after exclusion of the first 4 years of follow-up (HR, 1.25 [95% CI, 1.09-1.42]). Risk was inversely associated with intakes of yogurt (HR, 0.93 [95% CI, 0.89-0.98] per 100-g/d increment), cheese (HR, 0.92 [95% CI, 0.86-0.98] per 30-g/d increment), and eggs (HR, 0.93 [95% CI, 0.88-0.99] per 20-g/d increment); the associations with yogurt and eggs were attenuated and nonsignificant after exclusion of the first 4 years of follow-up. Risk was not significantly associated with intakes of poultry, fish, or milk. In analyses modeling dietary substitutions, replacement of 100 kcal/d from red and processed meat with 100 kcal/d from fatty fish, yogurt, cheese, or eggs was associated with ≈20% lower risk of IHD. Consumption of red and processed meat was positively associated with serum non-high-density lipoprotein cholesterol concentration and systolic blood pressure, and consumption of cheese was inversely associated with serum non-high-density lipoprotein cholesterol. Risk for IHD was positively associated with consumption of red and processed meat and inversely associated with consumption of yogurt, cheese, and eggs, although the associations with yogurt and eggs may be influenced by reverse causation bias. It is not clear whether the associations with red and processed meat and cheese reflect causality, but they were consistent with the associations of these foods with plasma non-high-density lipoprotein cholesterol and for red and processed meat with systolic blood pressure, which could mediate such effects.…
PMID: 31006335

Jordan Ovadia | ירדן עובדיה
דירוג זה מבוסס על 9 דוחות אימות קודמים.
האם הדוח הזה היה מועיל לך?
מה היה פחות טוב? (רשות)
תודה על הפידבק!
עירעור על דוח זה
ספקו ראיות חדשות או הצביעו על אי דיוקים
נעדכן אותך על תוצאות הבדיקה
הוסיפו קישורים למחקרים או מקורות רפואיים מוכרים
העירעור נשלח בהצלחה!
המנוע המדעי שלנו יבדוק את הראיות שהגשתם. נעדכן אתכם באימייל עם התוצאות.
ניתוח מבוסס בינה מלאכותית
דוח זה נוצר באופן אוטומטי על ידי מערכת בינה מלאכותית ועשוי להכיל שגיאות, אי-דיוקים או מידע חלקי. הניתוח אינו מהווה ייעוץ רפואי, אבחנה או המלצה לטיפול, והוא אינו תחליף לדעתו של איש מקצוע רפואי מוסמך. יש להתייעץ עם רופא או מומחה מוסמך לפני קבלת כל החלטה רפואית. המידע מוצג לצרכי מידע כללי בלבד.
מידע זה מופק על ידי בינה מלאכותית ואינו מהווה תחליף לייעוץ רפואי מקצועי.