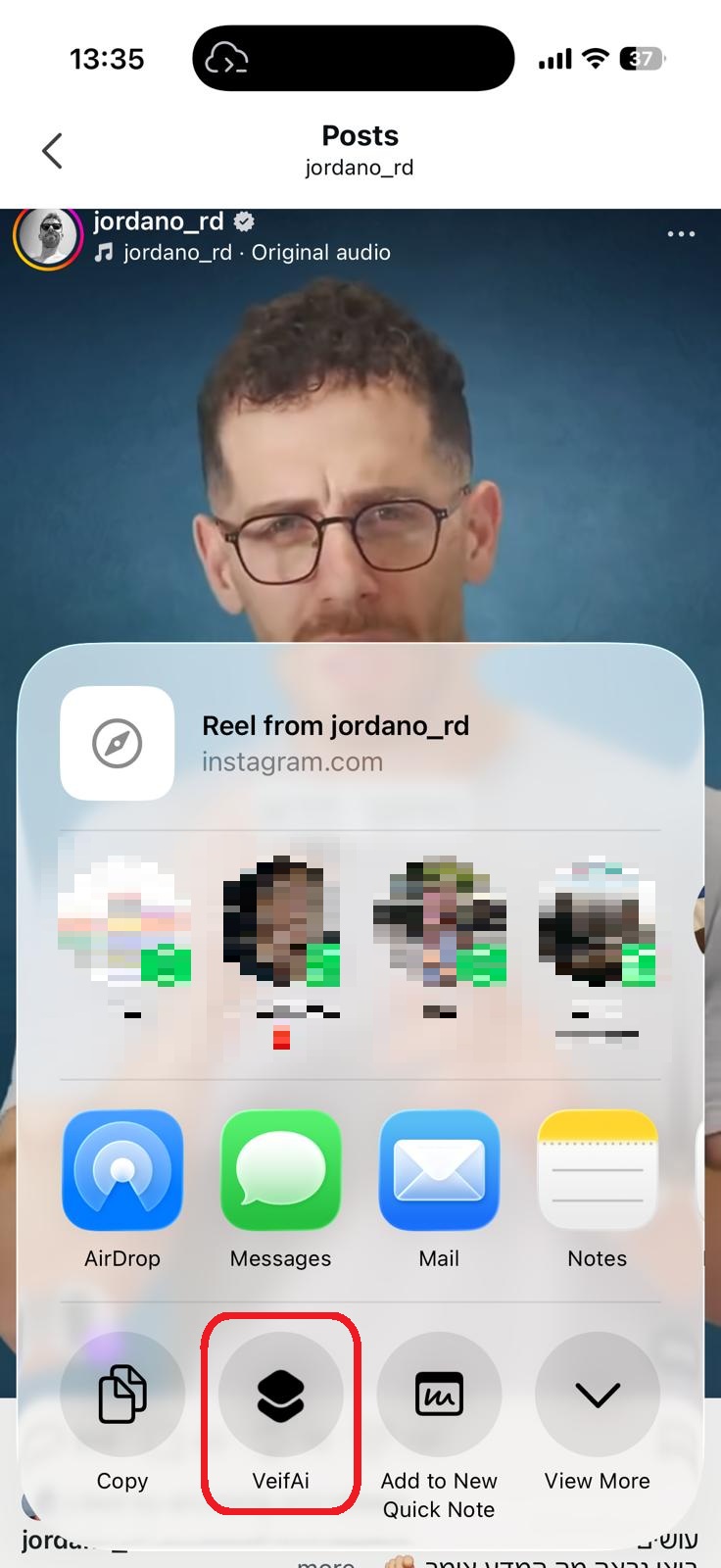
סריקה בתהליך...
הניתוח עשוי לארוך 30–90 שניות
הידעת?
הסרטון אינו מכיל תוכן רפואי
חושבים שחלה טעות?
אם לדעתכם הסרטון אכן עוסק בטענות רפואיות או בריאותיות, הוסיפו הסבר קצר ושלחו בקשה לבדיקה מחדש.
הבקשה התקבלה! נבדוק את הסרטון ונחזור אליכם.
אירעה שגיאה בשליחת הבקשה. נסו שוב.
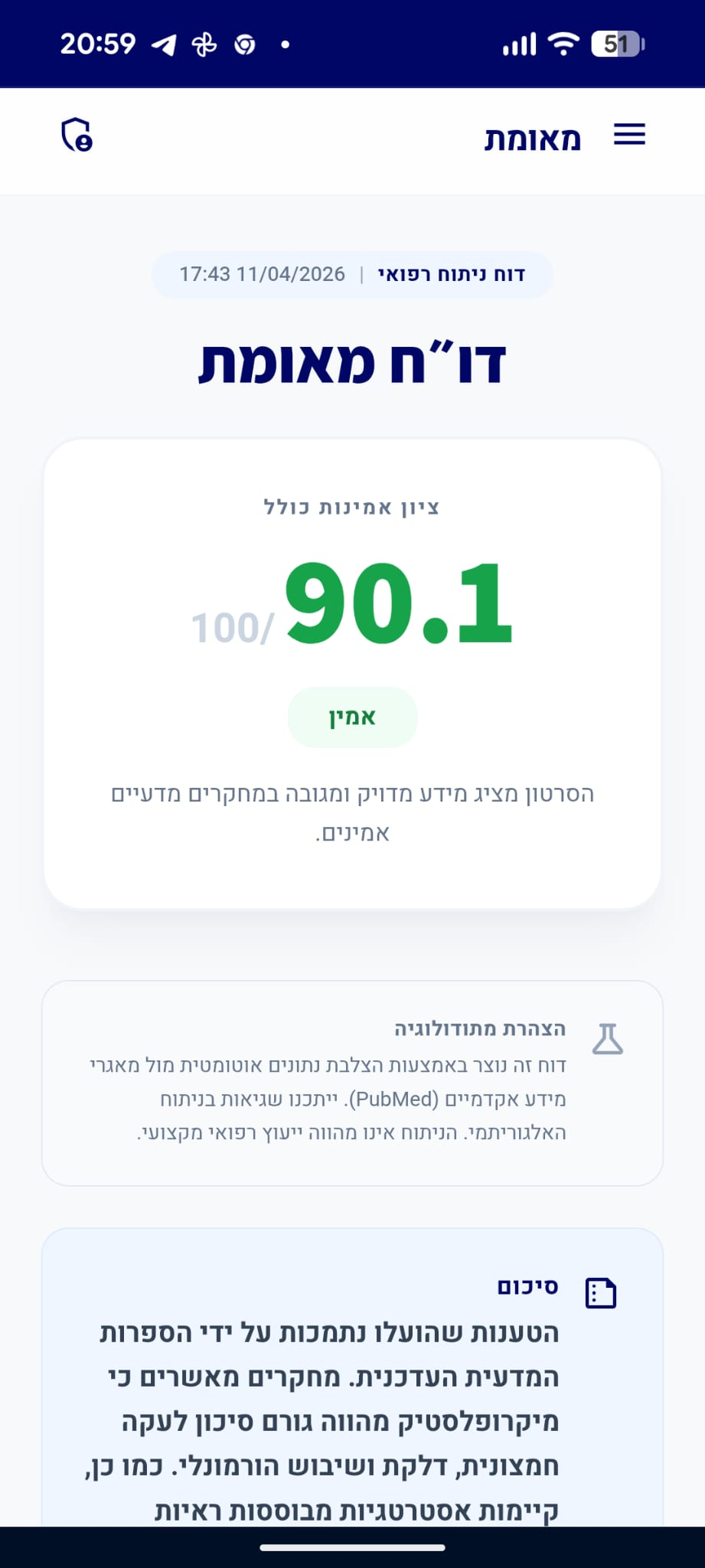
דו״ח מאומת
הסרטון מציג מידע מדויק ומגובה במחקרים מדעיים אמינים.
סיכום
הטענות שהועלו בנוגע לתדירות יציאות תקינה, הגורמים המשפיעים עליהן, הצורך בבירור רפואי במקרה של שינויים, ותפקידם של סיבים תזונתיים, נתמכות היטב על ידי הספרות המדעית וההנחיות הקליניות המקובלות. המידע המוצג עקבי עם הידע הרפואי הנוכחי.
analytics ניתוח טענות מבוסס ראיות
"טווח היציאות התקין נע בין פעם ביום ועד פעם ב-2-3 ימים."
מסקנת הבדיקה:
הספרות הרפואית מגדירה את טווח היציאות התקין באופן רחב, כאשר התדירות המקובלת נעה בין שלוש פעמים ביום לשלוש פעמים בשבוע. הטענה כי הטווח נע בין פעם ביום ל-2-3 ימים תואמת את הנורמות הקליניות המקובלות. (🟩)
"תדירות היציאות מושפעת מגורמים כמו תזונה, צריכת סיבים, שתייה, פעילות גופנית, סטרס וגנטיקה."
מסקנת הבדיקה:
קיימת הסכמה מדעית רחבה כי תדירות היציאות מושפעת ממגוון גורמים אורח חיים ופיזיולוגיים, כולל צריכת סיבים, נוזלים, רמת פעילות גופנית, גורמים פסיכולוגיים כגון סטרס, וגורמים גנטיים. (🟩)
chevron_right מקורות מדעיים: (3)
-
link
Understanding the physiology of human defaecation and disorders of continence and evacuation.
The act of defaecation, although a ubiquitous human experience, requires the coordinated actions of the anorectum and colon, pelvic floor musculature, and the enteric, peripheral and central nervous systems. Defaecation is best appreciated through the description of four phases, which are, temporally and physiologically, reasonably discrete. However, given the complexity of this process, it is unsurprising that disorders of defaecation are both common and problematic; almost everyone will experience constipation at some time in their life and many will develop faecal incontinence. A detailed understanding of the normal physiology of defaecation and continence is critical to inform management of disorders of defaecation. During the past decade, there have been major advances in the investigative tools used to assess colonic and anorectal function. This Review details the current understanding of defaecation and continence. This includes an overview of the relevant anatomy and physiology, a description of the four phases of defaecation, and factors influencing defaecation (demographics, stool frequency/consistency, psychobehavioural factors, posture, circadian rhythm, dietary intake and medications). A summary of the known pathophysiology of defaecation disorders including constipation, faecal incontinence and irritable bowel syndrome is also included, as well as considerations for further research in this field.…
PMID: 34373626
-
link
Association Between Stress Management Interventions and Symptom Severity in Adults With Irritable Bowel Syndrome (IBS) in Saudi Arabia.
<h4>Background</h4>Psychological stress is a major contributing factor to irritable bowel syndrome (IBS), a widespread functional gastrointestinal disorder. Consequently, understanding the relationship between stress management strategies and the severity of IBS symptoms is crucial.<h4>Aim</h4>This study sought to assess the association between stress management interventions and symptom severity among adults with IBS in Saudi Arabia. Furthermore, it investigated the associations between IBS, demographic data, lifestyle habits, and perceived stress levels.<h4>Methodology</h4>We conducted a cross-sectional study involving adults aged 18 and older in Saudi Arabia who had a clinical diagnosis of IBS. Participants completed a validated, bilingual web-based survey that incorporated the Rome IV diagnostic criteria, the IBS Symptom Severity Scale (IBS-SSS), and the Perceived Stress Scale (PSS). Statistical significance for both descriptive and inferential analyses was established at p < 0.05.<h4>Results</h4>The study included 517 participants, of whom 24% utilized stress management techniques. The most prevalent methods were deep breathing (66.9%), meditation (50.8%), and yoga (30.6%). Comparative analysis showed significantly lower symptom severity scores among those practicing stress management, specifically regarding the frequency of abdominal pain (p = 0.010), abdominal distension (p < 0.002), satisfaction with bowel habits (p < 0.001), and interference with daily activities (p = 0.007). Analysis indicated that individuals engaging in stress management reported fewer severe symptoms and lower perceived stress, whereas high stress levels were significantly more common among non-practitioners (p = 0.007). Gender and lifestyle choices were also significantly linked to IBS burden.<h4>Conclusion</h4>The use of stress management protocols is associated with reduced symptom severity and lower perceived stress in IBS patients. These results advocate for the integration of stress reduction techniques into comprehensive IBS care plans.…
PMID: 41769512
-
link
An Examination of Factors Affecting Bowel Preparation for Colonoscopy: A Meta-Analysis.
<h4>Background</h4>The accuracy of colonoscopy results is significantly affected by the quality of bowel preparation. Identifying and understanding the factors that contribute to effective bowel preparation are crucial for optimizing patient outcomes.<h4>Purpose</h4>The aim of this meta-analysis was to systematically evaluate the variables influencing bowel preparation efficacy in order to inform the development of improved clinical protocols and patient care strategies.<h4>Methods</h4>We conducted a literature search of several databases to find studies that investigated factors affecting the quality of bowel preparation over a period ranging from the inception of each database to November 5, 2024. Studies were independently screened based on preestablished inclusion and exclusion criteria. The meta-analysis was conducted using RevMan 5.4 software.<h4>Results</h4>The meta-analysis included 27 articles containing data from 30,716 patients who underwent bowel preparation for colonoscopy. Eight factors were identified that were significantly associated with suboptimal bowel preparation: older age (odds ratio [OR], 1.28; 95% CI, 1.12-1.68; P = 0.019), male gender (OR, 1.33; 95% CI, 1.16-1.53; P < 0.001), chronic constipation (OR, 3.46; 95% CI, 2.65-4.09; P < 0.001), diabetes (OR, 4.72; 95% CI, 2.18-10.22; P < 0.001), use of opioids (OR, 1.62; 95% CI, 1.24-2.45; P = 0.006), a preprocedure high-fiber diet (OR, 2.94; 95% CI, 1.65-5.22; P < 0.001), an interval exceeding five hours between the final administration of the bowel cleansing agent and the procedure (OR, 2.82; 95% CI, 1.79-4.45; P < 0.001), and a last bowel movement that is not watery (OR, 4.78; 95% CI, 2.35-9.71; P < 0.001).<h4>Conclusion</h4>Health care providers, including nurses, should consider these determinants of bowel preparation effectiveness and implement appropriate interventions in a timely manner to enhance patient education and care.…
PMID: 41566605
"יש לפנות לבירור רפואי במקרה של שינוי פתאומי בהרגלי היציאות, כאב בזמן יציאה או מאמץ חריג."
מסקנת הבדיקה:
שינוי פתאומי בהרגלי היציאות נחשב ל'דגל אדום' קליני המחייב בירור רפואי כדי לשלול פתולוגיות משמעותיות. כאב ומאמץ חריג הם תסמינים המצדיקים הערכה רפואית בהתאם להנחיות הקליניות המקובלות. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
Management of Gastrointestinal Symptoms in Parkinson's Disease.
Gastrointestinal (GI) dysfunction is a common and often underappreciated aspect of Parkinson's disease (PD), with symptoms manifesting at multiple levels of the digestive tract, from swallowing difficulties to challenges with defecation. These non-motor symptoms can be more debilitating than the hallmark motor impairments of PD, profoundly affecting patients' quality of life. The burden of GI issues in PD extends beyond discomfort, contributing to malnutrition, weight loss, and impaired medication absorption, which can exacerbate both motor and non-motor symptoms. Despite their clinical significance, GI symptoms are frequently overlooked or mismanaged in routine practice. Inappropriate treatments, including certain medications and dietary recommendations, may inadvertently worsen the disease course. Therefore, a comprehensive understanding of GI dysfunction in PD is critical for clinicians, especially neurologists, to optimize patient care. This review provides an updated overview of the common GI manifestations in PD, including drooling, dyspepsia and dysphagia, gastroparesis, constipation, Many people with Parkinson’s disease (PD) experience digestive problems, but these issues are often overlooked. Symptoms can affect the entire digestive system, from difficulty swallowing to trouble with bowel movements. In some cases, these problems can be more challenging than the movement difficulties caused by PD. Poor digestion can lead to malnutrition, weight loss, and problems absorbing medication, which may worsen both motor and non-motor symptoms. Unfortunately, digestive issues in PD are sometimes mismanaged, and certain treatments or dietary changes might make things worse. It is important for doctors to understand and properly address these symptoms. This article provides an updated overview of common digestive problems in PD, including drooling, difficulty swallowing, slow stomach emptying, constipation, and infections in the gut. It also discusses how these issues can be diagnosed and treated using both medical and non-medical approaches. Proper management of digestive problems can help improve the quality of life for people with PD.…
PMID: 40823476
-
link
Recent Developments in On-Demand Voiding Therapies.
One cannot survive without regularly urinating and defecating. People with neurologic injury (spinal cord injury, traumatic brain injury, stroke) or disease (multiple sclerosis, Parkinson's disease, spina bifida) and many elderly are unable to voluntarily initiate voiding. The great majority of them require bladder catheters to void urine and "manual bowel programs" with digital rectal stimulation and manual extraction to void stool. Catheter-associated urinary tract infections frequently require hospitalization, whereas manual bowel programs are time consuming (1 to 2 hours) and stigmatizing and cause rectal pain and discomfort. Laxatives and enemas produce defecation, but onset and duration are unpredictable, prolonged, and difficult to control, which can produce involuntary defecation and fecal incontinence. Patients with spinal cord injury (SCI) consider recovery of bladder and bowel function a higher priority than recovery of walking. Bladder and bowel dysfunction are a top reason for institutionalization of elderly. Surveys indicate that convenience, rapid onset and short duration, reliability and predictability, and efficient voiding are priorities of SCI individuals. Despite the severe, unmet medical need, there is no literature regarding on-demand, rapid-onset, short-duration, drug-induced voiding therapies. This article provides in-depth discussion of recent discovery and development of two candidates for on-demand voiding therapies. The first, [Lys…
PMID: 38641354
"סיבים תזונתיים מעלים את נפח הצואה ומשפרים את המרקם שלה, מה שמקל על היציאות."
מסקנת הבדיקה:
מחקרים רבים, כולל מטא-אנליזות, מאשרים כי סיבים תזונתיים תורמים להגדלת נפח הצואה ושיפור עקביותה, מה שמסייע בהקלה על עצירות ושיפור תפקוד המעי. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
Effect of dietary fiber on constipation: a meta analysis.
To investigate the effect of dietary fiber intake on constipation by a meta-analysis of randomized controlled trials (RCTs). We searched Ovid MEDLINE (from 1946 to October 2011), Cochrane Library (2011), PubMed for articles on dietary fiber intake and constipation using the terms: constipation, fiber, cellulose, plant extracts, cereals, bran, psyllium, or plantago. References of important articles were searched manually for relevant studies. Articles were eligible for the meta-analysis if they were high-quality RCTs and reported data on stool frequency, stool consistency, treatment success, laxative use and gastrointestinal symptoms. The data were extracted independently by two researchers (Yang J and Wang HP) according to the described selection criteria. Review manager version 5 software was used for analysis and test. Weighted mean difference with 95%CI was used for quantitative data, odds ratio (OR) with 95%CI was used for dichotomous data. Both I(2) statistic with a cut-off of ≥ 50% and the χ(2) test with a P value < 0.10 were used to define a significant degree of heterogeneity. We searched 1322 potential relevant articles, 19 of which were retrieved for further assessment, 14 studies were excluded for various reasons, five studies were included in the analysis. Dietary fiber showed significant advantage over placebo in stool frequency (OR = 1.19; 95%CI: 0.58-1.80, P < 0.05). There was no significant difference in stool consistency, treatment success, laxative use and painful defecation between the two groups. Stool frequency were reported by five RCTs, all results showed either a trend or a significant difference in favor of the treatment group, number of stools per week increased in treatment group than in placebo group (OR = 1.19; 95%CI: 0.58-1.80, P < 0.05), with no significant heterogeneity among studies (I(2)= 0, P = 0.77). Four studies evaluated stool consistency, one of them presented outcome in terms of percentage of hard stool, which was different from others, so we included the other three studies for analysis. Two studies reported treatment success. There was significant heterogeneity between the studies (P < 0.1, I(2) > 50%). Three studies reported laxative use, quantitative data was shown in one study, and the pooled analysis of the other two studies showed no significant difference between treatment and placebo groups in laxative use (OR = 1.07; 95%CI 0.51-2.25), and no heterogeneity was found (P = 0.84, I(2)= 0). Three studies evaluated painful defecation: one study presented both quantitative and dichotomous data, the other two studies reported quantitative and dichotomous data separately. We used dichotomous data for analysis. Dietary fiber intake can obviously increase stool frequency in patients with constipation. It does not obviously improve stool consistency, treatment success, laxative use and painful defecation.…
PMID: 23326148
-
link
Effects of β-Fructans Fiber on Bowel Function: A Systematic Review and Meta-Analysis.
The aim of this systematic review and meta-analysis was to assess the effects of β-fructan supplementation on bowel function in healthy volunteers and patients. The search process was based on the selection of publications listed in the Pubmed and EUPMC database until December 2017, plus two unpublished studies, to identify studies evaluating the impact of β-fructans on bowel movement and stool parameters. Forty-seven publications were selected for inclusion. Primary parameter was frequency of bowel movements, evaluated by the number of defecations per day during the study period. Secondary outcomes were stool consistency, stool dry and wet weights, and transit time. Short-chain (DP < 10) β-fructans contributed to increased stool frequency (0.36 defecation +/- 0.06 per day;…
PMID: 30621208
"עדיף לצרוך סיבים תזונתיים ממזון מלא (ירקות, פירות ודגנים מלאים) ולא מתוספים."
מסקנת הבדיקה:
הנחיות תזונתיות קליניות מדגישות את העדיפות לצריכת סיבים ממקורות מזון מלאים בשל הערך התזונתי המוסף (ויטמינים, מינרלים ופיטוכימיקלים) והשפעתם הסינרגטית על הבריאות, בהשוואה לתוספי סיבים מבודדים. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
Gut-Lung Axis in COPD: Investigating the Impact of Dietary Fiber Intake on Systemic Inflammation and Lung Function Decline.
<h4>Objective</h4>The gut-lung axis represents a promising therapeutic target in chronic obstructive pulmonary disease (COPD). This study investigated whether dietary fiber intake differs between COPD patients and healthy controls, and examined its association with systemic inflammation and lung function.<h4>Methods</h4>A case-control study was conducted including 100 COPD patients (cases) and 100 age- and sex-matched healthy controls. Dietary fiber intake was assessed using a validated food frequency questionnaire. Systemic inflammatory markers (CRP, IL-6) were measured by ELISA. Lung function parameters (FEV<sub>1</sub>, FEV<sub>1</sub>/FVC, DLCO) were evaluated according to ATS/ERS guidelines. Logistic regression analysis was performed to assess the association between dietary fiber intake and COPD risk.<h4>Results</h4>COPD patients had significantly lower dietary fiber intake (18.30 ± 6.20 g/day) compared to controls (28.70 ± 8.10 g/day, <i>P</i> < 0.001). Inflammatory markers were significantly elevated in COPD patients: CRP (5.80 ± 3.20 vs. 1.20 ± 0.80 mg/L), IL-6 (8.40 ± 4.10 vs. 2.10 ± 1.30 pg/mL) (all <i>P</i> < 0.001). In COPD patients, dietary fiber intake was inversely correlated with CRP (<i>r</i> = -0.52), IL-6 (<i>r</i> = -0.48), and positively correlated with FEV<sub>1</sub> (<i>r</i> = 0.41) and DLCO (<i>r</i> = 0.38) (all <i>P</i> < 0.001). After adjusting for confounders, low dietary fiber intake (<20 g/day) was associated with 3.2-fold increased odds of COPD (OR = 3.24, 95% CI: 1.86-5.65, <i>P</i> < 0.001).<h4>Conclusion</h4>Low dietary fiber intake is significantly associated with COPD and correlates with increased systemic inflammation and reduced lung function. These findings support the potential role of the gut-lung axis in COPD pathophysiology. However, causality cannot be established due to the limitations of the cross-sectional case-control design. Prospective interventional studies are warranted to confirm these associations and evaluate whether dietary fiber modification can improve clinical outcomes in COPD patients.…
PMID: 41878303
-
link
Perceived Barriers to Increased Whole Grain Consumption by Older Adults in Long-Term Care.
Many older adults fail to consume adequate amounts of dietary fiber from food sources, including whole grains. Little information is available about consumption of dietary fiber and whole grains by residents of long-term care facilities. Surveys were mailed to 3,000 randomly selected US members of the Academy of Nutrition and Dietetics who worked in practice groups related to elder care. Net response rate was 22.7% (n = 681). Cost was a barrier to whole grain use for 27.1% of respondents, followed by dietary needs (22.1%), contracts in place (20.3%), and overall nutritional content (20.1%). Over 75% of respondents stated their patients require dietary fiber supplementation. Nutrition professionals most frequently (23.6%) reported spending $11-20 monthly per patient on dietary fiber supplements. Although a majority of facilities served whole grain foods daily, 89.5% of respondents would like to serve more whole grains. Ready-to-eat cereals, bread, bagels, and hot cereals were the most common whole grain products served at the facilities where survey respondents worked. An economic analysis of the benefits of increased consumption of whole grains and other high-fiber foods versus the use of laxative supplements may be helpful to administrators of long-term care facilities.…
PMID: 29252145

Lior Ben Moshe | רפואה בשפה פשוטה
דירוג זה מבוסס על 1 דוחות אימות קודמים.
האם הדוח הזה היה מועיל לך?
מה היה פחות טוב? (רשות)
תודה על הפידבק!
עירעור על דוח זה
ספקו ראיות חדשות או הצביעו על אי דיוקים
נעדכן אותך על תוצאות הבדיקה
הוסיפו קישורים למחקרים או מקורות רפואיים מוכרים
העירעור נשלח בהצלחה!
המנוע המדעי שלנו יבדוק את הראיות שהגשתם. נעדכן אתכם באימייל עם התוצאות.
ניתוח מבוסס בינה מלאכותית
דוח זה נוצר באופן אוטומטי על ידי מערכת בינה מלאכותית ועשוי להכיל שגיאות, אי-דיוקים או מידע חלקי. הניתוח אינו מהווה ייעוץ רפואי, אבחנה או המלצה לטיפול, והוא אינו תחליף לדעתו של איש מקצוע רפואי מוסמך. יש להתייעץ עם רופא או מומחה מוסמך לפני קבלת כל החלטה רפואית. המידע מוצג לצרכי מידע כללי בלבד.
מידע זה מופק על ידי בינה מלאכותית ואינו מהווה תחליף לייעוץ רפואי מקצועי.