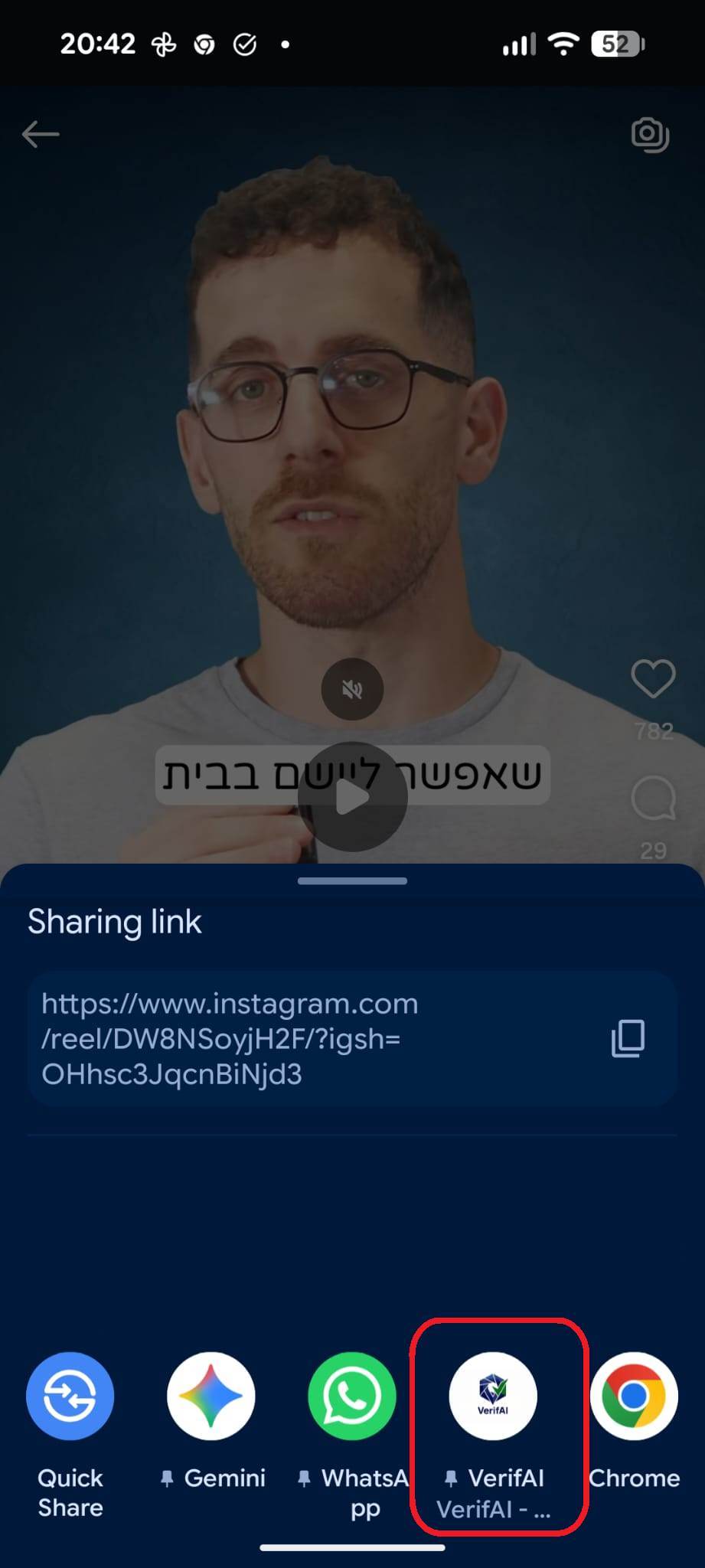
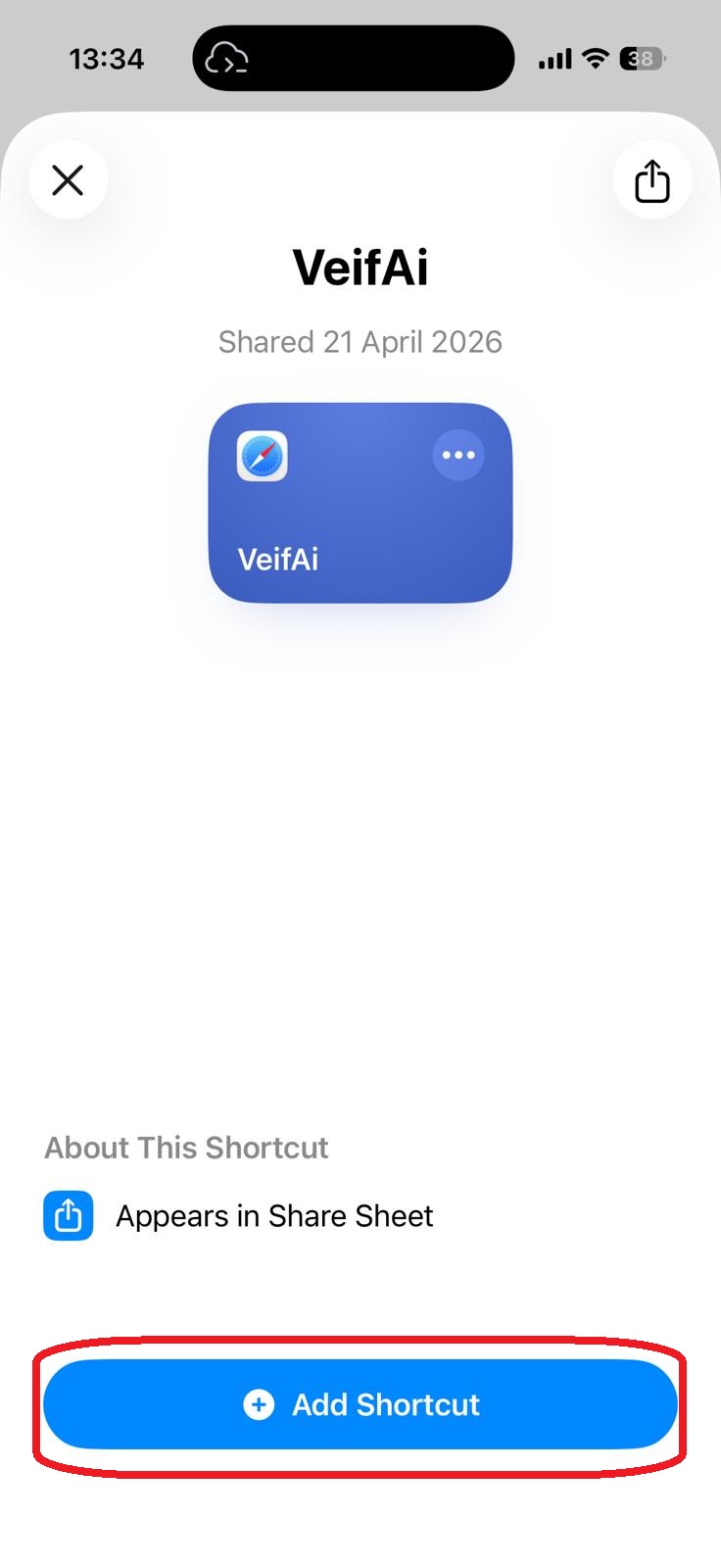
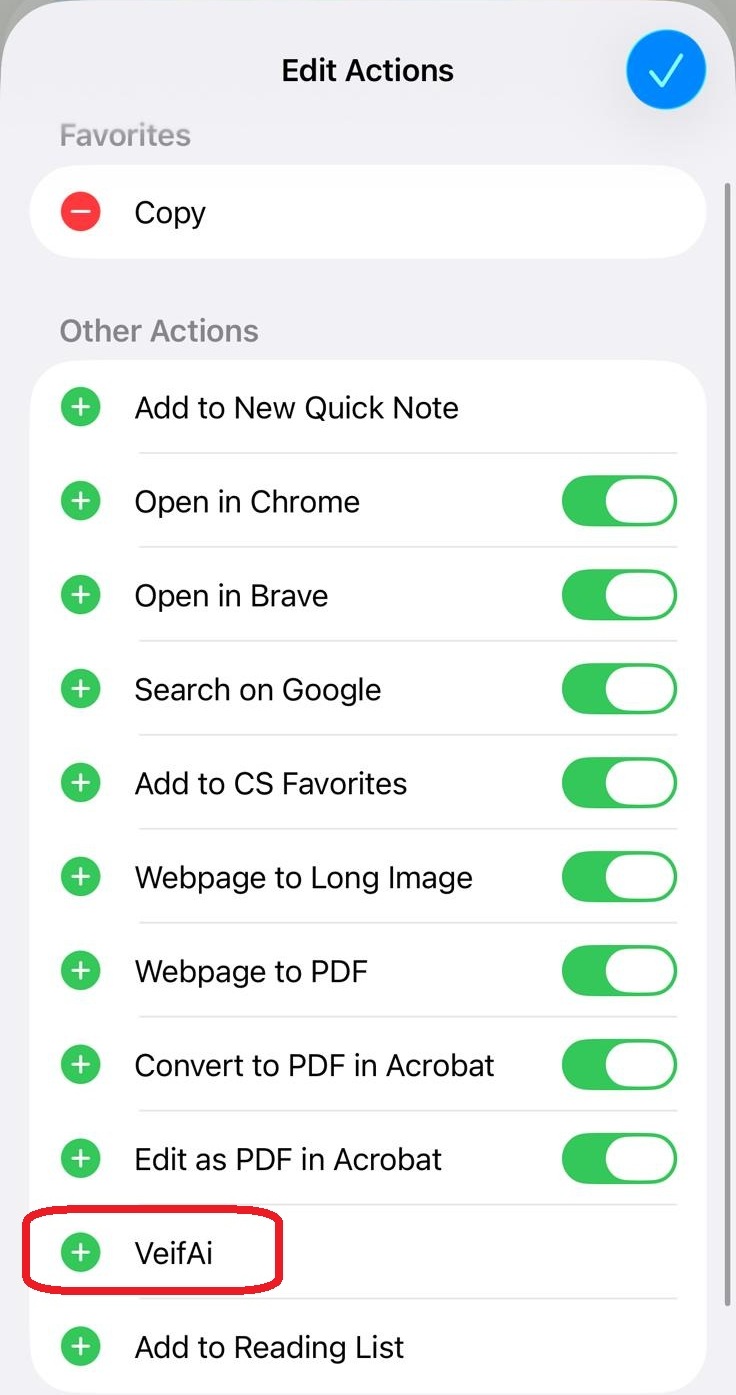
סריקה בתהליך...
הניתוח עשוי לארוך 30–90 שניות
הידעת?
הסרטון אינו מכיל תוכן רפואי
חושבים שחלה טעות?
אם לדעתכם הסרטון אכן עוסק בטענות רפואיות או בריאותיות, הוסיפו הסבר קצר ושלחו בקשה לבדיקה מחדש.
הבקשה התקבלה! נבדוק את הסרטון ונחזור אליכם.
אירעה שגיאה בשליחת הבקשה. נסו שוב.
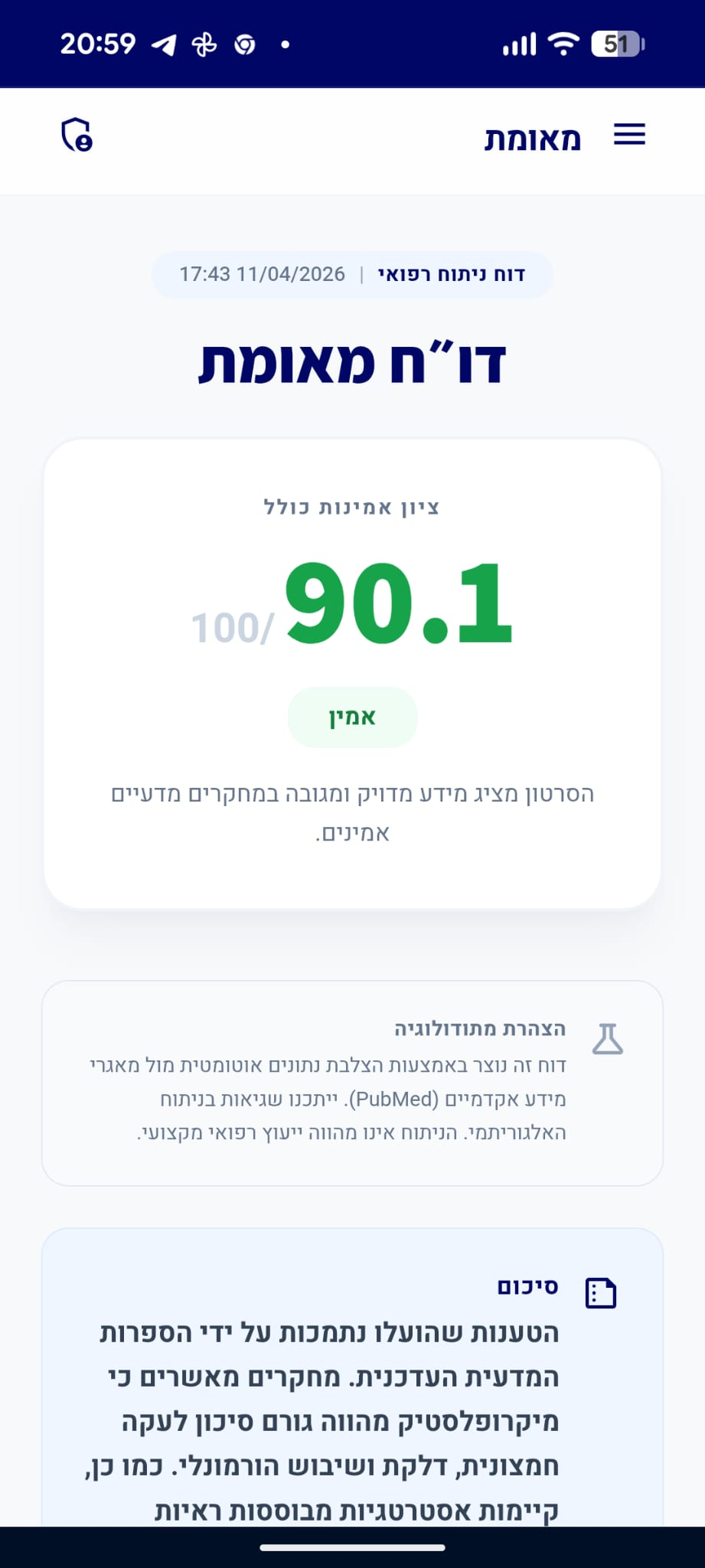
דו״ח מאומת
הדוח קיבל עירעור ונמצא כעת בבדיקה מחודשת. הציון יעודכן בסיום הבדיקה.
⚠️ דוח בבדיקה מחודשת
דוח זה אותגר לדיוק. המנוע המדעי שלנו מעריך מחדש את הטענות על בסיס ראיות חדשות שהוגשו.
סיכום
רוב הטענות בסרטון מבוססות על פוטנציאל תיאורטי או מחקרי ראשוני (in vitro), אך חסרות ביסוס קליני מוצק בבני אדם. בנוסף, הטענה לגבי בריאות הלב סותרת את העובדה המוכרת כי שמן קוקוס מעלה את רמות הכולסטרול ה-LDL.
analytics ניתוח טענות מבוסס ראיות
"שמן קוקוס מסייע במניעת פטריית הקנדידה וחיידק ההליקובקטר פילורי"
מסקנת הבדיקה:
קיימות עדויות מחקריות על פוטנציאל אנטי-בקטריאלי של חומצה קפרילית (הנמצאת בשמן קוקוס) נגד הליקובקטר פילורי במעבדה, אך אין הוכחה קלינית מבוססת לכך שצריכת השמן מונעת זיהומים אלו בבני אדם. (🟨)
"צריכת שמן קוקוס מסייעת בתהליך שריפת השומן בגוף"
מסקנת הבדיקה:
בעוד שחומצות שומן בינוניות-שרשרת עוברות מטבוליזם שונה משומנים ארוכי-שרשרת, אין ראיות חותכות לכך ששמן קוקוס כשלעצמו גורם לשריפת שומן מוגברת או לירידה במשקל בבני אדם. (🟨)
"שמן קוקוס עשוי לסייע במניעת מחלות ניווניות כמו דמנציה ואלצהיימר"
מסקנת הבדיקה:
קיימת השערה מדעית כי גופי קטון המופקים מחילוף חומרים של שמן קוקוס עשויים לספק אנרגיה חלופית למוח, אך אין הוכחות קליניות חותכות לכך שצריכתו מונעת דמנציה או אלצהיימר. (🟨)
chevron_right מקורות מדעיים: (3)
-
link
Alzheimer's Disease and Type 2 Diabetes Mellitus: The Use of MCT Oil and a Ketogenic Diet.
Recently, type 2 diabetes mellitus (T2DM) has been reported to be strongly associated with Alzheimer's disease (AD). This is partly due to insulin resistance in the brain. Insulin signaling and the number of insulin receptors may decline in the brain of T2DM patients, resulting in impaired synaptic formation, neuronal plasticity, and mitochondrial metabolism. In AD patients, hypometabolism of glucose in the brain is observed before the onset of symptoms. Amyloid-β accumulation, a main pathology of AD, also relates to impaired insulin action and glucose metabolism, although ketone metabolism is not affected. Therefore, the shift from glucose metabolism to ketone metabolism may be a reasonable pathway for neuronal protection. To promote ketone metabolism, medium-chain triglyceride (MCT) oil and a ketogenic diet could be introduced as an alternative source of energy in the brain of AD patients.…
PMID: 34830192
-
link
The role of dietary coconut for the prevention and treatment of Alzheimer's disease: potential mechanisms of action.
Coconut, Cocos nucifera L., is a tree that is cultivated to provide a large number of products, although it is mainly grown for its nutritional and medicinal values. Coconut oil, derived from the coconut fruit, has been recognised historically as containing high levels of saturated fat; however, closer scrutiny suggests that coconut should be regarded more favourably. Unlike most other dietary fats that are high in long-chain fatty acids, coconut oil comprises medium-chain fatty acids (MCFA). MCFA are unique in that they are easily absorbed and metabolised by the liver, and can be converted to ketones. Ketone bodies are an important alternative energy source in the brain, and may be beneficial to people developing or already with memory impairment, as in Alzheimer's disease (AD). Coconut is classified as a highly nutritious 'functional food'. It is rich in dietary fibre, vitamins and minerals; however, notably, evidence is mounting to support the concept that coconut may be beneficial in the treatment of obesity, dyslipidaemia, elevated LDL, insulin resistance and hypertension - these are the risk factors for CVD and type 2 diabetes, and also for AD. In addition, phenolic compounds and hormones (cytokinins) found in coconut may assist in preventing the aggregation of amyloid-β peptide, potentially inhibiting a key step in the pathogenesis of AD. The purpose of the present review was to explore the literature related to coconut, outlining the known mechanistic physiology, and to discuss the potential role of coconut supplementation as a therapeutic option in the prevention and management of AD.…
PMID: 25997382
-
link
Impact of Coconut Oil and Its Bioactive Metabolites in Alzheimer's Disease and Dementia: A Systematic Review and Meta-Analysis.
<b>Background/Objectives</b>: Alzheimer's disease (AD) is the most common form of dementia and affects approximately 50 million individuals worldwide. Interest in coconut oil (CO) as a potential dietary intervention has surged owing to its substantial medium-chain triglyceride (MCT) content. Therefore, sustaining cognitive function and potentially slowing the progression of AD are crucial. This systematic review and meta-analysis evaluated the effects of CO and its bioactive metabolites on AD and dementia. <b>Methods</b>: The review protocol is registered in PROSPERO (CRD42023450435). Relevant research articles published between January 2015 and June 2023 were systematically searched. Seven studies met the predetermined eligibility criteria. Thematic analysis was utilized to synthesis the data about the qualitative features, while meta-analysis was employed for the quantitative findings. A meta-analysis was conducted to assess the standardized mean difference (SMD) and the corresponding 95% confidence interval (CI). Forest plots were generated using Review Manager 5.3 (RevMan 5.3). <b>Results</b>: The analysis revealed that all studies showed consistent results regarding the effects of CO on cognitive scores, with little variability in the true effects of CO on cognitive scores across the studies included in the meta-analysis. <b>Conclusions</b>: CO improved cognitive scores in patients with AD compared with those in the control group (<i>p</i> < 0.05). The results of this study add to the increasing amount of evidence indicating that MCTs found in CO might be a way to improve abilities and potentially slow the advancement of AD. The findings of this study may encourage the development of targeted dietary strategies and interventions for individuals at risk of or diagnosed with AD.…
PMID: 39589946
"לשמן קוקוס מיוחסות תכונות אנטי-סרטניות"
מסקנת הבדיקה:
מחקרים מצביעים על מנגנונים אנטי-סרטניים פוטנציאליים של חומצה לאורית במעבדה, אך לא קיימות הוכחות קליניות לכך שצריכת שמן קוקוס מונעת סרטן בבני אדם. (🟨)
"צריכת שמן קוקוס תורמת לשמירה על בריאות הלב"
מסקנת הבדיקה:
הטענה ששמן קוקוס בריא ללב שנויה במחלוקת עזה; מחקרים מראים כי הוא מעלה את רמות ה-LDL (הכולסטרול ה'רע'), מה שעלול להגביר סיכון קרדיווסקולרי ולא להפחיתו. (🟨)
chevron_right מקורות מדעיים: (4)
-
link
Impact of coconut oil consumption on cardiovascular health: a systematic review and meta-analysis.
Coconut oil is rich in medium-chain fatty acids and has been claimed to have numerous health benefits. This review aimed to examine the evidence surrounding coconut oil consumption and its impact on cardiovascular health. A systematic literature search of the PubMed, Embase, the Cochrane Library, and CINAHL databases, up to May 2019, was performed. Study characteristics including study design, population, intervention, comparator, outcome, and source of funding were summarized. Meta-analyses included 12 studies to provide estimates of effects. Subgroup analyses were performed to account for any differences in the study-level characteristics. When compared with plant oils and animal oils, coconut oil was found to significantly increase high-density lipoprotein cholesterol (HDL-C) by 0.57 mg/dL (95%CI, 0.40-0.74 mg/dL; I2 = 6.7%) and 0.33 mg/dL (0.01-0.65 mg/dL; I2 = 0%), respectively. Coconut oil significantly raised low-density lipoprotein cholesterol (LDL-C) by 0.26 mg/dL (0.09-0.43 mg/dL; I2 = 59.7%) compared with plant oils and lowered LDL-C (-0.37 mg/dL; -0.69 to -0.05 mg/dL; I2 = 48.1%) compared with animal oils. No significant effects on triglyceride were observed. Better lipid profiles were demonstrated with the virgin form of coconut oil. Compared with animal oils, coconut oil demonstrated a better lipid profile n comparison with plant oils, coconut oil significantly increased HDL-C and LDL-C.…
PMID: 31769848
-
link
Coconut oil consumption and cardiovascular risk factors in humans.
Coconut oil is being heavily promoted as a healthy oil, with benefits that include support of heart health. To assess the merits of this claim, the literature on the effect of coconut consumption on cardiovascular risk factors and outcomes in humans was reviewed. Twenty-one research papers were identified for inclusion in the review: 8 clinical trials and 13 observational studies. The majority examined the effect of coconut oil or coconut products on serum lipid profiles. Coconut oil generally raised total and low-density lipoprotein cholesterol to a greater extent than cis unsaturated plant oils, but to a lesser extent than butter. The effect of coconut consumption on the ratio of total cholesterol to high-density lipoprotein cholesterol was often not examined. Observational evidence suggests that consumption of coconut flesh or squeezed coconut in the context of traditional dietary patterns does not lead to adverse cardiovascular outcomes. However, due to large differences in dietary and lifestyle patterns, these findings cannot be applied to a typical Western diet. Overall, the weight of the evidence from intervention studies to date suggests that replacing coconut oil with cis unsaturated fats would alter blood lipid profiles in a manner consistent with a reduction in risk factors for cardiovascular disease.…
PMID: 26946252
-
link
The Effect of Coconut Oil Consumption on Cardiovascular Risk Factors: A Systematic Review and Meta-Analysis of Clinical Trials.
Coconut oil is high in saturated fat and may, therefore, raise serum cholesterol concentrations, but beneficial effects on other cardiovascular risk factors have also been suggested. Therefore, we conducted a systematic review of the effect of coconut oil consumption on blood lipids and other cardiovascular risk factors compared with other cooking oils using data from clinical trials. We searched PubMed, SCOPUS, Cochrane Registry, and Web of Science through June 2019. We selected trials that compared the effects of coconut oil consumption with other fats that lasted at least 2 weeks. Two reviewers independently screened articles, extracted data, and assessed the study quality according to the PRISMA guidelines (Preferred Reporting Items for Systematic Reviews and Meta-Analyses). The main outcomes included low-density lipoprotein cholesterol (LDL-cholesterol), high-density lipoprotein cholesterol (HDL-cholesterol), total cholesterol, triglycerides, measures of body fatness, markers of inflammation, and glycemia. Data were pooled using random-effects meta-analysis. 16 articles were included in the meta-analysis. Results were available from all trials on blood lipids, 8 trials on body weight, 5 trials on percentage body fat, 4 trials on waist circumference, 4 trials on fasting plasma glucose, and 5 trials on C-reactive protein. Coconut oil consumption significantly increased LDL-cholesterol by 10.47 mg/dL (95% CI: 3.01, 17.94; Coconut oil consumption results in significantly higher LDL-cholesterol than nontropical vegetable oils. This should inform choices about coconut oil consumption.…
PMID: 31928080
-
link
Randomised trial of coconut oil, olive oil or butter on blood lipids and other cardiovascular risk factors in healthy men and women.
High dietary saturated fat intake is associated with higher blood concentrations of low-density lipoprotein cholesterol (LDL-C), an established risk factor for coronary heart disease. However, there is increasing interest in whether various dietary oils or fats with different fatty acid profiles such as extra virgin coconut oil may have different metabolic effects but trials have reported inconsistent results. We aimed to compare changes in blood lipid profile, weight, fat distribution and metabolic markers after four weeks consumption of 50 g daily of one of three different dietary fats, extra virgin coconut oil, butter or extra virgin olive oil, in healthy men and women in the general population. Randomised clinical trial conducted over June and July 2017. General community in Cambridgeshire, UK. Volunteer adults were recruited by the British Broadcasting Corporation through their websites. Eligibility criteria were men and women aged 50-75 years, with no known history of cancer, cardiovascular disease or diabetes, not on lipid lowering medication, no contraindications to a high-fat diet and willingness to be randomised to consume one of the three dietary fats for 4 weeks. Of 160 individuals initially expressing an interest and assessed for eligibility, 96 were randomised to one of three interventions; 2 individuals subsequently withdrew and 94 men and women attended a baseline assessment. Their mean age was 60 years, 67% were women and 98% were European Caucasian. Of these, 91 men and women attended a follow-up assessment 4 weeks later. Participants were randomised to extra virgin coconut oil, extra virgin olive oil or unsalted butter and asked to consume 50 g daily of one of these fats for 4 weeks, which they could incorporate into their usual diet or consume as a supplement. The primary outcome was change in serum LDL-C; secondary outcomes were change in total and high-density lipoprotein cholesterol (TC and HDL-C), TC/HDL-C ratio and non-HDL-C; change in weight, body mass index (BMI), waist circumference, per cent body fat, systolic and diastolic blood pressure, fasting plasma glucose and C reactive protein. LDL-C concentrations were significantly increased on butter compared with coconut oil (+0.42, 95% CI 0.19 to 0.65 mmol/L, P<0.0001) and with olive oil (+0.38, 95% CI 0.16 to 0.60 mmol/L, P<0.0001), with no differences in change of LDL-C in coconut oil compared with olive oil (-0.04, 95% CI -0.27 to 0.19 mmol/L, P=0.74). Coconut oil significantly increased HDL-C compared with butter (+0.18, 95% CI 0.06 to 0.30 mmol/L) or olive oil (+0.16, 95% CI 0.03 to 0.28 mmol/L). Butter significantly increased TC/HDL-C ratio and non-HDL-C compared with coconut oil but coconut oil did not significantly differ from olive oil for TC/HDL-C and non-HDL-C. There were no significant differences in changes in weight, BMI, central adiposity, fasting blood glucose, systolic or diastolic blood pressure among any of the three intervention groups. Two different dietary fats (butter and coconut oil) which are predominantly saturated fats, appear to have different effects on blood lipids compared with olive oil, a predominantly monounsaturated fat with coconut oil more comparable to olive oil with respect to LDL-C. The effects of different dietary fats on lipid profiles, metabolic markers and health outcomes may vary not just according to the general classification of their main component fatty acids as saturated or unsaturated but possibly according to different profiles in individual fatty acids, processing methods as well as the foods in which they are consumed or dietary patterns. These findings do not alter current dietary recommendations to reduce saturated fat intake in general but highlight the need for further elucidation of the more nuanced relationships between different dietary fats and health. NCT03105947; Results.…
PMID: 29511019

Healme טיפוח טבעי | יוצרת תוכן
דירוג זה מבוסס על 4 דוחות אימות קודמים.
האם הדוח הזה היה מועיל לך?
מה היה פחות טוב? (רשות)
תודה על הפידבק!
עירעור על דוח זה
ספקו ראיות חדשות או הצביעו על אי דיוקים
נעדכן אותך על תוצאות הבדיקה
הוסיפו קישורים למחקרים או מקורות רפואיים מוכרים
העירעור נשלח בהצלחה!
המנוע המדעי שלנו יבדוק את הראיות שהגשתם. נעדכן אתכם באימייל עם התוצאות.
ניתוח מבוסס בינה מלאכותית
דוח זה נוצר באופן אוטומטי על ידי מערכת בינה מלאכותית ועשוי להכיל שגיאות, אי-דיוקים או מידע חלקי. הניתוח אינו מהווה ייעוץ רפואי, אבחנה או המלצה לטיפול, והוא אינו תחליף לדעתו של איש מקצוע רפואי מוסמך. יש להתייעץ עם רופא או מומחה מוסמך לפני קבלת כל החלטה רפואית. המידע מוצג לצרכי מידע כללי בלבד.
מידע זה מופק על ידי בינה מלאכותית ואינו מהווה תחליף לייעוץ רפואי מקצועי.