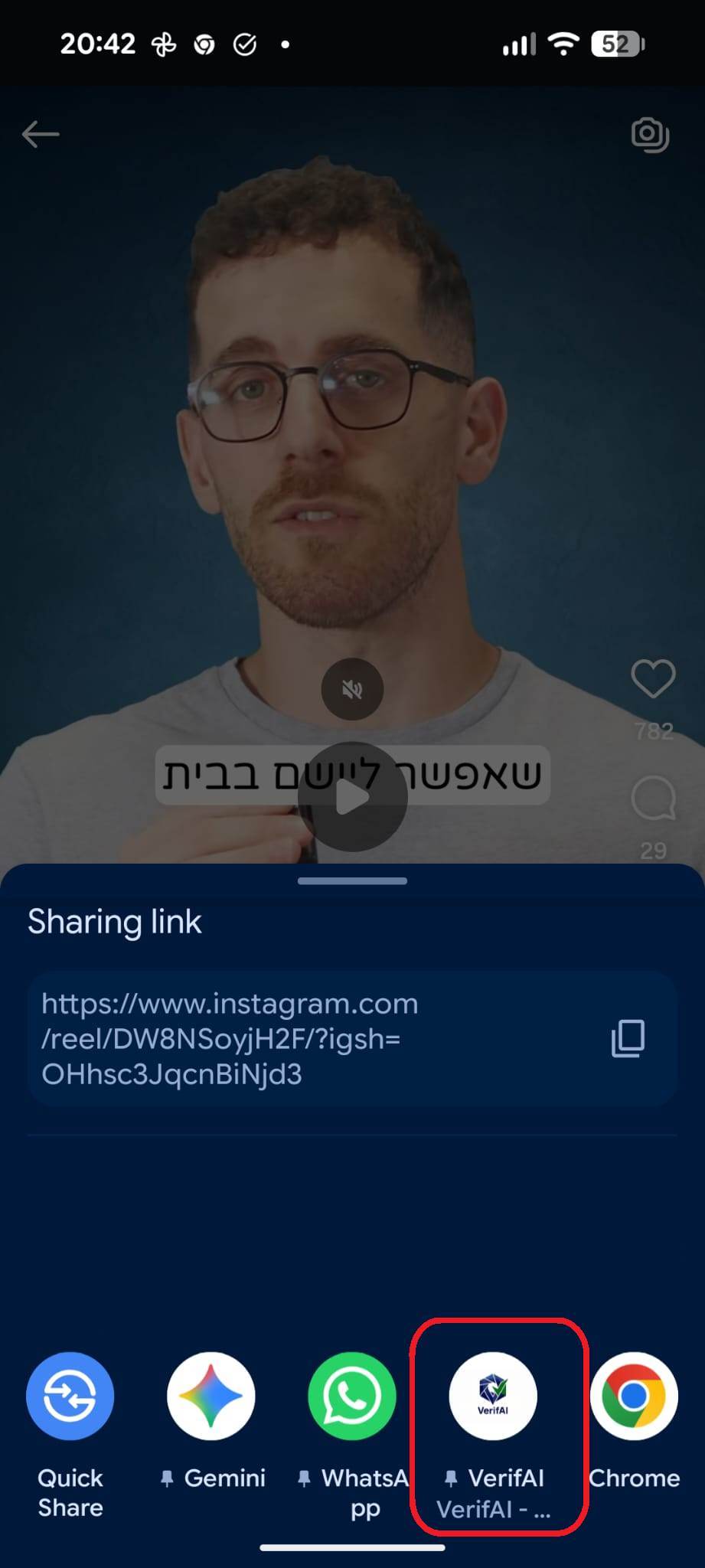
סריקה בתהליך...
הניתוח עשוי לארוך 30–90 שניות
הידעת?
הסרטון אינו מכיל תוכן רפואי
חושבים שחלה טעות?
אם לדעתכם הסרטון אכן עוסק בטענות רפואיות או בריאותיות, הוסיפו הסבר קצר ושלחו בקשה לבדיקה מחדש.
הבקשה התקבלה! נבדוק את הסרטון ונחזור אליכם.
אירעה שגיאה בשליחת הבקשה. נסו שוב.
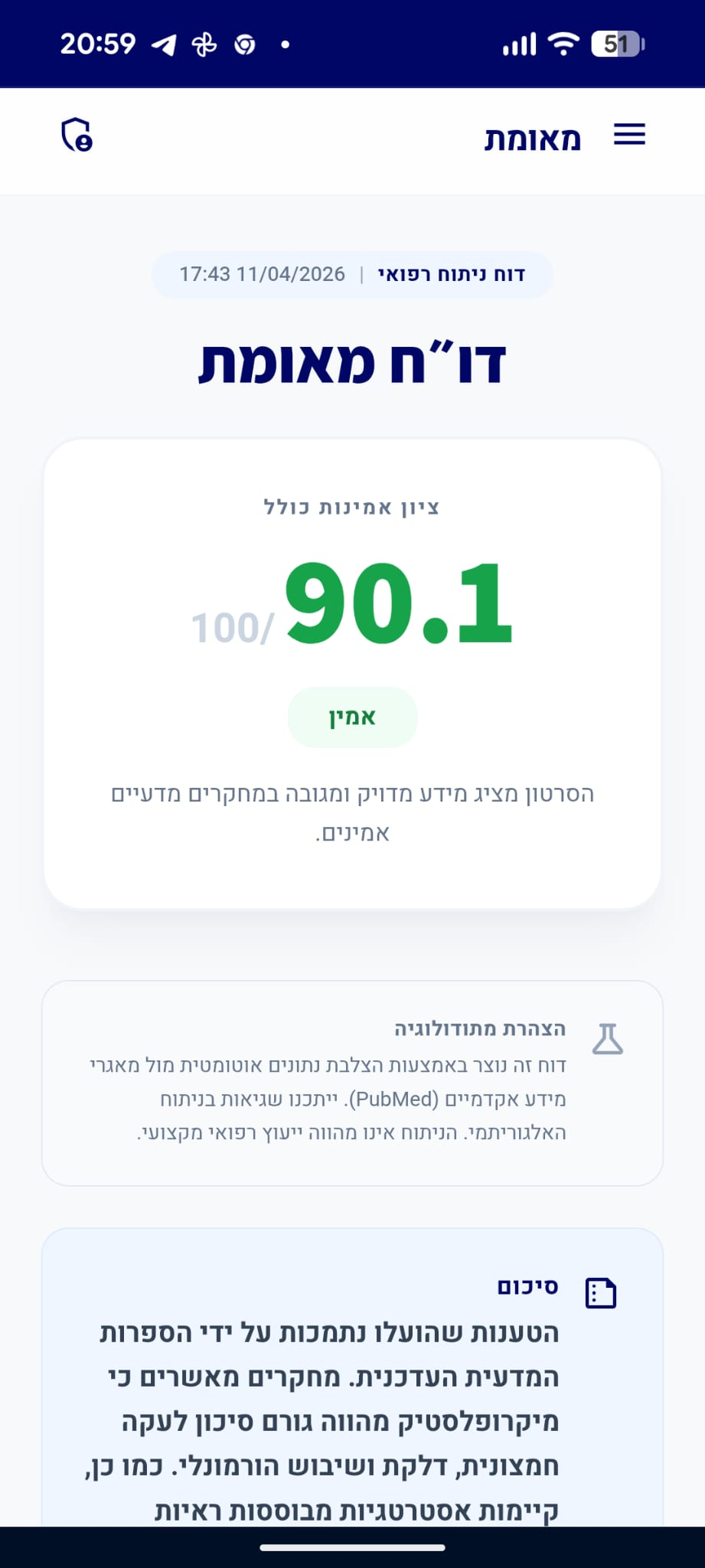
דו״ח מאומת
הסרטון מציג מידע מדויק ומגובה במחקרים מדעיים אמינים.
סיכום
כל הטענות שהועלו נמצאו מאומתות על ידי הספרות המדעית. קיים קשר מוכח בין שתן חומצי לתסמיני שלפוחית רגיזה, כאשר המנגנון הפיזיולוגי מערב תעלות TRP. כמו כן, הוכח כי התערבות תזונתית (פירות וירקות) או טיפול תרופתי בבסיס (סודה לשתייה) יכולים להעלות את ה-pH של השתן ולשפר את התסמינים הקליניים.
analytics ניתוח טענות מבוסס ראיות
"שתן חומצי קשור לשלפוחית רגיזה (OAB)."
מסקנת הבדיקה:
מחקרים קליניים, כגון PMID 25766740, מראים קשר מובהק בין שתן חומצי לבין תסמיני שלפוחית רגיזה (OAB), כאשר אחוז משמעותי מהחולים מציגים רמות pH נמוכות. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
The Relationship between Acidic Urinary pH and Overactive Bladder; Alkalization of Urine Improves the Symptoms of Overactive Bladder.
To determine association between urine pH and OAB symptoms and to determine if urinary alkalization improves overactive bladder (OAB) symptoms. 659 patients with OAB were enrolled in this study between June 2012 and May 2014. 329 patients (group 1) were included in the final analysis. 201 adults were used as a control group (group 2). 24-hour urinary pH and the validated Turkish version of the OAB-V8 questionnaire were performed in patients. A 24-hour urine pH <6.2 was considered acidic urine. In the second part, a diet program was performed for 4 weeks in 30 participants. Urine pH values and OAB-V8 scoring results were recorded before the diet program and 2 and 4 weeks after the diet program. Acidic urinary pH was determined in 61.4% of patients with OAB. There was a significant association between the presence of acidic urine and OAB. Also, the OAB-V8 scores of patients were significantly higher in patients with acidic urine than nonacidic urine. OAB-V8 scores of patients showed statistically significant improvement after diet therapy (17.87 ± 6.52 vs. 10.43 ± 7.17; p < 0.001). We found that acidic urinary pH was closely associated with OAB, and alkalization of urine improved lower urinary tract symptoms. We suggest that urinary pH should be considered as a parameter in treatment planning of patients with OAB.…
PMID: 25766740
-
link
The Role of Acidic Urine on Detrusor Pressure in Patients with Overactive Bladder: A Urodynamic Evaluation.
To evaluate the relationship between urine pH value and urodynamic parameters in patients with overactive bladder. The patients' data whose underwent standard urodynamic study at two tertiary centers in our city. The period between January 2015-January 2021 was reviewed retrospectively. The inclusion criteria were the patients with overactive bladder, over 18 years of age, and with urine analysis before urodynamic study. Patients were divided into two groups as those with acidic urine pH (Group 1) and without (Group 2). The detrusor pressures obtained from filling cystometry were compared between the groups. In addition, the correlation between detrusor pressure and urine pH was examined. The data from 211 patients (109 females, 102 males) were analyzed during the screening period. Eighty-two patients were in Group 1 and 129 patients in Group 2. The mean age was similar between the groups ( The presence of acidic urinalysis is associated with many urodynamic findings. Significantly, the patients with detrusor overactivity had more acidic urine than without detrusor overactivity. Therefore, for patients with high detrusor pressure, urinalysis should be evaluated carefully.…
PMID: 36330571
"שתן חומצי גורם לגירוי בשלפוחית השתן דרך תעלות TRP, מה שיוצר דחף להשתין."
מסקנת הבדיקה:
תעלות TRP (כגון TRPV1) ידועות כחיישנים המגיבים לשינויי pH וגירויים כימיים בשלפוחית השתן, מה שמוביל להפעלת עצבים תחושתיים ולתחושת דחף להשתנה. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
TRP Channels as Lower Urinary Tract Sensory Targets.
Several members of the transient receptor potential (TRP) superfamily, including TRPV1, TRPV2, TRPV4, TRM4, TRPM8 and TRPA1, are expressed in the lower urinary tract (LUT), not only in neuronal fibers innervating the bladder and urethra, but also in the urothelial and muscular layers of the bladder and urethral walls. In the LUT, TRP channels are mainly involved in nociception and mechanosensory transduction. Animal studies have suggested the therapeutic potential of several TRP channels for the treatment of both bladder over- and underactivity and bladder pain disorders,; however translation of this finding to clinical application has been slow and the involvement of these channels in normal human bladder function, and in various pathologic states have not been established. The development of selective TRP channel agonists and antagonists is ongoing and the use of such agents can be expected to offer new and important information concerning both normal physiological functions and possible therapeutic applications.…
PMID: 31121962
-
link
Physiological functions and pharmacological targeting of transient receptor potential channels.
Transient receptor potential (TRP) channels represent an extensive and diverse protein family fulfilling salient roles as versatile cellular sensors and effectors. The pivotal role of TRP and related ion channels in sensory processes has been well documented. Over the last few years, a new concept has emerged that TRP proteins control an exceptionally broad spectrum of homeostatic physiological functions such as maintenance of body temperature, blood pressure, transmitter release from neurons, mineral and energy homeostasis, and reproduction. This notion is further supported by more than 20 hereditary human diseases in areas as diverse as neurology, cardiology, hematology, pulmonology, nephrology, dermatology, and urology. Most TRP channel-related human disorders impinge on development, metabolism, and other homeostatic functions. The remarkable diversity of pathologies caused by TRP channel dysfunction underscores these proteins' broad spectrum of roles in vivo. Here, we provide a comprehensive overview of our progress in the identification, characterization, and clinical relevance of pharmacological agents targeting mammalian TRP channels. SIGNIFICANCE STATEMENT: Accumulating evidence links transient receptor potential (TRP) channels to various human diseases and highlights TRPs as the most appealing pharmacological targets. The review provides an overview of this quickly developing research area, focusing on identified pharmacological modulators of mammalian TRP channels.…
PMID: 41118703
"בסיס השתן (למשל באמצעות סודה לשתייה) יכול לשפר את תסמיני השלפוחית הרגיזה."
מסקנת הבדיקה:
מספר מחקרים קליניים מבוקרים הדגימו כי טיפול בבסיס (כגון סודה לשתייה) להעלאת ה-pH של השתן מפחית משמעותית את תסמיני השלפוחית הרגיזה אצל מטופלים עם שתן חומצי. (🟩)
chevron_right מקורות מדעיים: (3)
-
link
Comparison of Oral Sodium Bicarbonate and Solifenacin Treatment in Female Overactive Bladder Patients With Acidic Urine pH.
In this study, we planned to compare the effects of oral sodium bicarbonate (NaHCO3) and anticholinergic (solifenacin) treatments in women with overactive bladder (OAB) and acidic urine pH values (<6). According to the referral order of OAB patients, 8 g/d oral NaHCO3 (group 1) or 5 mg/d solifenacin succinate (group 2) was given to the patients. Both treatment regimens were applied one at a time for 12 weeks in total. Laboratory values, bladder diary, Patient Perception of Bladder Condition score, Patient Perception of Intensity of Urgency Scale, Overactive Bladder-Validated 8-Question Awareness Tool, and the King's Health Questionnaire (KHQ) scores before and after treatment were compared. A total of 59 patients were evaluated. Thirty-one patients were included in group 1, and 28 patients were included in group 2. No difference was detected in pretreatment and posttreatment laboratory values other than urine pH values in both groups. Whereas there was no difference in pretreatment urine pH values among the 2 groups, posttreatment urine pH values were significantly higher in group 1 compared with group 2 (P = 0.08, P < 0.001, respectively). There was a significant amelioration in the bladder diary parameters, symptom scores, and KHQ values measured after treatment in both groups. However, degree of amelioration in posttreatment outcomes was similar among the groups. It was demonstrated that urinary alkalization made with oral NaHCO3 in female OAB patients with acidic urine pH had a significantly positive effect on symptoms and symptom scores, and these results are similar to the results of solifenacin treatment.…
PMID: 30335650
-
link
Effects of urine alkalinization with sodium bicarbonate orally on lower urinary tract symptoms in female patients: a pilot study.
In this study, we planned to explore the effects of sodium bicarbonate orally (NaHCO3) treatment on female patients with lower urinary tract symptoms (LUTS) who have acidic urine pH values (<6). NaHCO3 was given orally to 33 female patients for 4 weeks at a dose of 2 × 4 g/day. Laboratory values, bladder diary, the Patient Perception of Bladder Condition Score (PPBC), Patient Perception of Intensity of Urgency Scale (PPIUS), Overactive Bladder-Validated 8-question Awareness tool (OAB-V8), Pelvic Pain and Urgency & Frequency Patient Symptom Scale tests (PUFSS), and the King's Health Questionnaire (KHQ) scores before and after treatment were compared. A significant increase was detected in urine pH values measured after treatment (5.31 ± 0.52 to 7.2 ± 0.66, p < 0.001), but not in blood pH values (7.369 ± 0.33 to 7.384 ± 0.28, p = 0.14). After treatment, a significant decrease was detected in daily frequency, nocturia, urgency, and urge incontinence prevalence (p < 0.001,p = 0.003, p < 0.001, p = 0.002, respectively) and PPBC, PPIUS, PUFSS, and OAB-V8 symptom scores (p = 0.004, p = 0.002, p < 0.001, p < 0.001, respectively). A significant decrease was detected in all KHQ subunit scores. Urine alkalinization with NaHCO3 orally in female patients with LUTS and acidic urine pH has a significant level of positive effects on symptoms and symptom scores. Our results show that this new treatment modality-which is inexpensive, easy to use, and has a low side-effect profile is effective in this chronic patient group.…
PMID: 28975365
-
link
The Relationship between Acidic Urinary pH and Overactive Bladder; Alkalization of Urine Improves the Symptoms of Overactive Bladder.
To determine association between urine pH and OAB symptoms and to determine if urinary alkalization improves overactive bladder (OAB) symptoms. 659 patients with OAB were enrolled in this study between June 2012 and May 2014. 329 patients (group 1) were included in the final analysis. 201 adults were used as a control group (group 2). 24-hour urinary pH and the validated Turkish version of the OAB-V8 questionnaire were performed in patients. A 24-hour urine pH <6.2 was considered acidic urine. In the second part, a diet program was performed for 4 weeks in 30 participants. Urine pH values and OAB-V8 scoring results were recorded before the diet program and 2 and 4 weeks after the diet program. Acidic urinary pH was determined in 61.4% of patients with OAB. There was a significant association between the presence of acidic urine and OAB. Also, the OAB-V8 scores of patients were significantly higher in patients with acidic urine than nonacidic urine. OAB-V8 scores of patients showed statistically significant improvement after diet therapy (17.87 ± 6.52 vs. 10.43 ± 7.17; p < 0.001). We found that acidic urinary pH was closely associated with OAB, and alkalization of urine improved lower urinary tract symptoms. We suggest that urinary pH should be considered as a parameter in treatment planning of patients with OAB.…
PMID: 25766740
"צריכת פירות וירקות מסייעת בהעלאת רמת ה-pH של השתן (הפחתת חומציות)."
מסקנת הבדיקה:
צריכת פירות וירקות מעלה את רמת ה-pH בשתן בשל תכולת המינרלים הבסיסיים (כמו אשלגן ומגנזיום) המנוגדים לחומציות המטבולית, עובדה המוכרת בספרות התזונתית והאורולוגית. (🟩)
chevron_right מקורות מדעיים: (2)
-
link
Popular Diets and Kidney Stones.
Popular diets often influence dietary patterns, which have different implications for kidney stone risk. Despite the wide variety of popular diets, some general principles can be gleaned from investigating their potential impact on nephrolithiasis. Plant-based diets, including Dietary Approaches to Stop Hypertension, Mediterranean, flexitarian, and vegetarian diets, may protect against nephrolithiasis when they consist largely of unprocessed plant foods, while carbohydrate-restricted diets (including high-protein diets and the ketogenic diet) may raise kidney stone risk. Patients should be advised to consume a diet rich in whole plants, particularly fruits and vegetables, and minimize their consumption of animal proteins. Accompanying fruits and vegetables that are higher in oxalate content with more water and some dairy intake may also be useful. (We address the oxalate content of fruits and vegetables further below). Calcium consumption is an important component of decreasing the risk of kidney stones, as higher dietary calcium from dairy or nondairy sources is independently associated with lower kidney stone risk. Patients should also be advised to be conscious of fat intake, as fat in the intestinal lumen may complex with calcium and therefore increase urinary oxalate excretion. Finally, patients should avoid consumption of processed foods, which often contain added fructose and high sodium content, two factors that increase kidney stone risk.…
PMID: 38453270
-
link
Dietetic and lifestyle recommendations for stone formers.
Nutrition is tightly associated with the risk of stone events. A part from genetic predisposition, a correct and balanced diet might prevent incident kidney stones. Several studies analyzed each dietary component and different diets to better understand their impact on stone recurrence. Fluids: High fluids intake is the most important factor for preventing kidney stones disease and for every 200 mL of water, the risk of stones is reduced by 13%. Soft drinks seems to be associated to a greater risk of stone events, whereas caffeine and citrus fruits juice are not. Calcium: Normally calcium intake with diet does not exceed 1.2 g/day. A balanced consumption of dairy products is capable of reducing oxalate intestinal absorption and urinary excretion compared to low calcium diet, being protective for stone disease. Oxalate: The exact amount of oxalate contained in different foods is difficult to estimate for its variability, even in the same aliment. In addition, the amount of oxalate consumed was shown to be only a minor risk factor for stone disease, whereas its intestinal absorption is strongly influenced by external factors, such as calcium intake. Dietary oxalate restriction is advisable only in patients with known elevated consumption. Sodium: High sodium intake is both associated with hypertension, heart disease and stone risk. Increased sodium consumption is directly associated to hypercalciuria in both calcium stone formers and healthy subjects. Although dietary sodium restriction to recommended values is always desirable in stone formers, it is difficult to achieve for its broad use in food preparation. Proteins: Animal proteins are associated to increased risk for stone formation, whereas vegetable and dairy proteins are not. Increased meat intake was associated to acidic urine pH, negative calcium balance and reduced anti-lithogenic urinary solutes excretion.Fruits and vegetables: Alkalizing foods are one of the most important factors for stone protection. Their consumption increases anti-lithogenic solutes as citrate, potassium and magnesium. A diet rich in fruits and vegetables is strongly recommended for stone formers. Uric acid: Elevated meat consumption is either associated to increased purine metabolism and acid load, favoring uric acid nephrolithiasis by reducing urine pH and increasing urinary excretion of uric acid, especially in patients affected by metabolic syndrome and diabetes.In conclusion, the most effective diet for stone protection is rich in fruits and vegetables, low in animal proteins and salt, with balanced dairy product consumption and obviously, with elevated fluid intake. These characteristics make vegetarian and Mediterranean diets protective and useful for stone formers, whereas western diet is at risk for stone formation. La nutrición está fuertemente asociada al riesgo de episodios litiásicos. Aparte de la predisposición genética, una dieta correcta y balanceada podría prevenir la incidencia de litiasis renal. Varios estudios han analizado cada componente de la dieta y diferentes dietas para entender mejor su impacto sobre la recurrencia litiásica. Líquidos: Una alta ingesta de fluidos es el factor más importante para la prevención de la enfermedad litiásicay por cada 200 mL de agua, el riesgo de litiasis se reduce un 13%. Los refrescos parecen estar asociados a un mayor riesgo de eventos litiásicos, mientras que la cafeina y los zumos de cítricos no lo están. Calcio: Normalmente la ingesta diaria de calcio con la dieta no excede los 1,2 g. Un consumo balanceado de productos lácteos es capaz de reducir la absorción intestinal y la excreción urinaria de oxalato si lo comparamos con una dieta pobre en calcio, siendo protector para la enfermedad litiásica. Oxalato: La cantidad exacta de oxalato en las diferentes comidas es difícil de estimar debido a su variabilidad, incluso en el mismo alimento. Además, se demostró que la cantidad de oxalato ingerido era solo un factor de riesgo menor para la enfermedad litiásica, mientras que su absorción intestinal está fuertemente influenciada por factores externos como la ingesta de calcio. La restricción de oxalato en la dieta se aconseja solamente en pacientes con aumento probado en su consumo. Sodio: Una ingesta elevada de sodio se asocia tanto con la hipertensión como con la enfermedad cardiaca y el riesgo de litiasis. El consumo elevado de sodio está directamente asociado con la hipercalciuria, tanto en litiásicos cálcicos como en sujetos sanos. Aunque la restricción dietética de sodio a los valores recomendadoses deseable en los pacientes litiásicos, es difícil de conseguir debido al alto uso de sodio en la preparación de las comidas.Proteinas: Las proteinas animales están asociadas a un riesgo aumentado para la formación de litiasis, mientras que las vegetales y las de productos lácteos no. Un aumento de consumo de carne se ha asociado a un pH urinario ácido, balance de calcio negativo y reducciónde la excrección urinaria de solutos anti-litogénicos.Frutas y vegetales: Las comidas alcalinizantes son uno de los factores más importantes para la protección ante la litiasis. Su consumo aumenta los solutos anti-litogénicos como el citrato, potasio y magnesio. Una dieta rica en frutas y vegetales es muy recomendable para los pacientes litiásicos. Acido úrico: Un consumo elevado de carne está asociado tanto a un aumento de metabolismo de las purinas como a la carga ácida, favoreciendo la nefrolitiasis úrica al reducir el pH urinario y aumentar la excreción urinaria de ácido úrico, especialmente en pacientes afectados por el síndrome metabólico y diabetes.En conclusión, la dieta más efectiva para proteger contrala litiasis es la rica en frutas y vegetales, pobre en proteinas animales y sal, con un consumo balanceado de productos lácteos y, obviamente, con una alta ingesta de líquidos. Estas características hacen que las dietas vegetarianas y la mediterránea sean protectoras y útiles para los pacientes litiásicos, mientras que la dieta occidental sea una dieta de riesgo para la formación de litiasis.…
PMID: 33459627

The Seven Fat Cows חמאה גראס פד - שומן טאלו - אנימל בייסד
דירוג זה מבוסס על 1 דוחות אימות קודמים.
האם הדוח הזה היה מועיל לך?
מה היה פחות טוב? (רשות)
תודה על הפידבק!
עירעור על דוח זה
ספקו ראיות חדשות או הצביעו על אי דיוקים
נעדכן אותך על תוצאות הבדיקה
הוסיפו קישורים למחקרים או מקורות רפואיים מוכרים
העירעור נשלח בהצלחה!
המנוע המדעי שלנו יבדוק את הראיות שהגשתם. נעדכן אתכם באימייל עם התוצאות.
ניתוח מבוסס בינה מלאכותית
דוח זה נוצר באופן אוטומטי על ידי מערכת בינה מלאכותית ועשוי להכיל שגיאות, אי-דיוקים או מידע חלקי. הניתוח אינו מהווה ייעוץ רפואי, אבחנה או המלצה לטיפול, והוא אינו תחליף לדעתו של איש מקצוע רפואי מוסמך. יש להתייעץ עם רופא או מומחה מוסמך לפני קבלת כל החלטה רפואית. המידע מוצג לצרכי מידע כללי בלבד.
מידע זה מופק על ידי בינה מלאכותית ואינו מהווה תחליף לייעוץ רפואי מקצועי.